Identifying Predictors of Treatment Dropout Using ML Analysis of Motivational Interviewing Processes and Attachment‑Related Avoidance
Keywords:
Treatment Dropout, Machine Learning, Motivational Interviewing, Attachment Avoidance, Therapeutic AllianceAbstract
Objective: This study aimed to utilize advanced machine learning algorithms to evaluate whether baseline attachment-related avoidance and specific linguistic frequencies of client change talk and sustain talk during early Motivational Interviewing sessions can reliably predict subsequent outpatient psychotherapeutic treatment dropout.
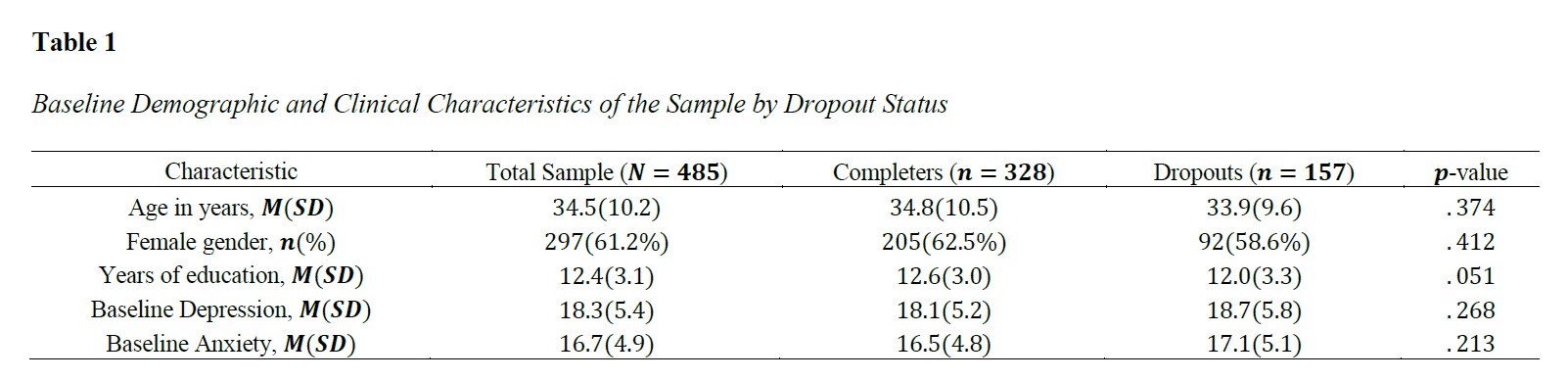
Methods and Materials: The study employed a prospective, longitudinal observational design with a sample of N=485 adults from Mexico City. Dropout was defined as missing three consecutive sessions or mutually agreeing to terminate prematurely. Data collection included baseline demographics, the Experiences in Close Relationships-Revised questionnaire to assess attachment-related avoidance, and Motivational Interviewing Skill Code ratings derived from the audio-recorded and transcribed first two therapy sessions. Machine learning analysis incorporated k-nearest neighbors imputation, Synthetic Minority Over-sampling Technique (SMOTE) for class imbalance, and evaluated Random Forest, Support Vector Machines (SVM), and Extreme Gradient Boosting (XGBoost) classifiers using stratified 10-fold cross-validation. SHapley Additive exPlanations (SHAP) values were utilized for model interpretability.
Findings: Results indicated that 157out of 485participants (32.4%) dropped out of treatment. Bivariate analyses revealed that dropouts had significantly higher attachment-related avoidance (M=4.25) compared to completers (M=3.15). During early sessions, the dropout cohort exhibited significantly more Sustain Talk (M=24.6 vs. M=15.2) and less Change Talk (M=19.8 vs. M=31.4), alongside receiving fewer complex reflections and lower empathy ratings from therapists. The XGBoost model demonstrated superior predictive performance (AUC=0.87), followed by Random Forest (AUC=0.84) and SVM (AUC=0.78). SHAP analyses identified attachment avoidance and patient sustain talk as the strongest overall predictors, highlighting a critical interaction effect where highly avoidant patients receiving fewer therapist complex reflections exhibited a compounding probability of dropout.
Conclusion: Machine learning algorithms can accurately predict treatment dropout from early clinical interactions, emphasizing that patient retention fundamentally depends on the complex interplay between severe attachment-related avoidance and the therapist’s technical proficiency in managing resistance.
Downloads
References
Ahmadi, A., & Raeisi, Z. (2018). The Effect of Acceptance and Commitment Therapy on Distress Tolerance in Mothers of Children with Autism [Research]. Quarterly Journal of Child Mental Health, 5(3), 69-79. http://childmentalhealth.ir/article-1-349-en.html
Banham, J. A., & Schweitzer, R. D. (2016). Trainee-therapists are not all equal: Examination of therapeutic efficiency, effectiveness and early client dropout after 12 months of clinical training. Psychology and Psychotherapy, 89(2), 148-162. https://doi.org/10.1111/papt.12071
Bentley, K. H., Cohen, Z. D., Kim, T., Bullis, J. R., Nauphal, M., Cassiello-Robbins, C., Sauer-Zavala, S., Sbi, S., Gallagher, M. W., Farchione, T. J., & Barlow, D. H. (2021). The Nature, Timing, and Symptom Trajectories of Dropout From Transdiagnostic and Single-Diagnosis Cognitive-Behavioral Therapy for Anxiety Disorders. Behavior therapy, 52(6), 1364-1376. https://doi.org/10.1016/j.beth.2021.03.007
Cortes, B., Ballesteros, A., Collantes, J., & Aguilar, M. L. (2016). What makes for good outcomes in solution-focused brief therapy? A follow-up study. European Psychiatry, 33(S1), s232-s233. https://doi.org/10.1016/j.eurpsy.2016.01.580
Daughters, S. B., Stipelman, B. A., Sargeant, M. N., Schuster, R., Bornovalova, M. A., & Lejuez, C. W. (2024). The interactive effects of antisocial personality disorder and court-mandated status on substance abuse treatment dropout. Journal of Substance Abuse Treatment, 34(2), 157-164. https://doi.org/10.1016/j.jsat.2007.02.007
Dickhaut, V., & Arntz, A. (2014). Combined group and individual schema therapy for borderline personality disorder: A pilot study. Journal of Behavior Therapy and Experimental Psychiatry, 45(2), 242-251. https://doi.org/10.1016/j.jbtep.2013.11.004
Gersh, E., Hallford, D. J., Rice, S. M., Kazantzis, N., Gersh, H., Gersh, B., & McCarty, C. A. (2017). Systematic review and meta-analysis of dropout rates in individual psychotherapy for generalized anxiety disorder. Journal of anxiety disorders, 52, 25-33. https://doi.org/10.1016/j.janxdis.2017.10.001
Giesen-Bloo, J., van Dyck, R., Spinhoven, P., van Tilburg, W., Dirksen, C., van Asselt, T., Kremers, I., Nadort, M., & Arntz, A. (2006). Outpatient Psychotherapy for Borderline Personality Disorder: Randomized Trial of Schema-Focused Therapy vs Transference-Focused Psychotherapy. Archives of General Psychiatry, 63(6), 649-658. https://doi.org/10.1001/archpsyc.63.6.649
Kliem, S., Kröger, C., & Kosfelder, J. (2010). Dialectical behavior therapy for borderline personality disorder: A meta-analysis using mixed-effects modeling. Journal of consulting and clinical psychology, 78(6), 936-951. https://doi.org/10.1037/a0021015
Kröger, C., Harbeck, S., Armbrust, M., & Kliem, S. (2013). Effectiveness, response, and dropout of dialectical behavior therapy for borderline personality disorder in an inpatient setting. Behaviour Research and Therapy, 51(8), 411-416. https://www.sciencedirect.com/science/article/pii/S0005796713000752
Kurt, Y. (2025). Attachment and Borderline Personality Features: The Mediating Roles of Hypomentalizing and Epistemic Mistrust. Clinical Psychology & Psychotherapy, 32(6). https://doi.org/10.1002/cpp.70185
Lammers, M. W., Vroling, M. S., Crosby, R. D., & van Strien, T. (2022). Dialectical behavior therapy compared to cognitive behavior therapy in binge-eating disorder: An effectiveness study with 6-month follow-up. International Journal of Eating Disorders, 55(7), 902-913. https://doi.org/10.1002/eat.23750
Lang, C. M., Edwards, A. J., Mittler, M. A., & Bonavitacola, L. (2018). Dialectical Behavior Therapy With Prolonged Exposure for Adolescents: Rationale and Review of the Research. Cognitive and Behavioral Practice, 25(3), 416-426. https://doi.org/10.1016/j.cbpra.2017.12.005
Leeuwerik, T., Cavanagh, K., & Strauss, C. (2019). Patient adherence to cognitive behavioural therapy for obsessive-compulsive disorder: A systematic review and meta-analysis. Journal of anxiety disorders, 68, 102135. https://doi.org/10.1016/j.janxdis.2019.102135
Linehan, M. M., Korslund, K. E., Harned, M. S., Gallop, R. J., Lungu, A., Neacsiu, A. D., McDavid, J., Comtois, K. A., & Murray-Gregory, A. M. (2015). Dialectical Behavior Therapy for High Suicide Risk in Individuals With Borderline Personality Disorder: A Randomized Clinical Trial and Component Analysis. JAMA Psychiatry, 72(5), 475-482. https://doi.org/10.1001/jamapsychiatry.2014.3039
Mansouri, K., & Khodabakhshi-Koolaee, A. (2024). The Effectiveness of Motivational Interview (MI) on Aggression and High-risk Behaviors of Adolescent Girls. JPEN, 10(4), 41-49. https://civilica.com/doc/2029606/
Miller, W. R. (2023). The Evolution of Motivational Interviewing. Behavioural and Cognitive Psychotherapy, 51(6), 616-632. https://doi.org/10.1017/s1352465822000431
Miller, W. R., & Rollnick, S. (2023). Motivational interviewing: Helping people change. Guilford Press. https://psycnet.apa.org/record/2012-17300-000
Mohammadi, M., Shirafkan-Kopekan, A., Shafiabadi, A., & Farhangi, A. (2025). The effectiveness of schema therapy on attachment styles and marital intimacy in couples in Tehran. Women Fam Stud Q, 17(64), 173-195. https://srb.sanad.iau.ir/en/Article/954007
Nejatifar, S., & Abedi, A. (2023). Effectiveness of Motivational Interviewing on Participation and Emotional Skills in Learning Disabled Adults. Psychological Research in Individuals with Exceptional Needs, 1(1), 32-40. https://doi.org/10.61838/kman.prien.1.1.5
Nielsen, S. K. K., Stuart, A. C., Winding, C., Pedersen, M. Ø., Franksdatter Daniel, S. I., Vangkilde, S., Rosenberg, N., & Hageman, I. (2025). Adult attachment style, emotion regulation and obsessive-compulsive disorder-A preliminary cross-sectional mediational investigation of an attachment-based model. Clinical Psychology & Psychotherapy, 32(1), e70031. https://doi.org/10.1002/cpp.70031
Pagan, A. F. (2024). Motivational Interviewing for Young Adults With Autism Spectrum Disorder: A Pilot Feasibility Study. https://doi.org/10.31234/osf.io/mt247
Parsafar, A. (2024). Investigating the Effectiveness of Motivational Interviewing on Social Anxiety and Academic Procrastination Among Students. Jayps, 5(3), 55-64. https://doi.org/10.61838/kman.jayps.5.3.6
Peterson, B. D., & Eifert, G. H. (2011). Using Acceptance and Commitment Therapy to Treat Infertility Stress. Cognitive and Behavioral Practice, 18(4), 577-587. https://doi.org/10.1016/j.cbpra.2010.03.004
Pudelko, A. H., Ramos, B., Emond, M., Péloquin, K., & Daspe, M. È. (2025). Is Our Attachment Hurting Us? Unraveling the Associations Between Partners' Attachment Pairings, Negative Emotions During Conflict, and Intimate Partner Violence. Journal of marital and family therapy, 51(2). https://doi.org/10.1111/jmft.70009
Rezaei, Z., Abolghasemi, S., Khalatbari, J., & Zarbakhsh, R. (2023). The effectiveness of a training package based on motivational interviewing, therapy based on acceptance and commitment, and therapy focused on compassion on tolerance of failure and health anxiety in patients with multiple sclerosis. Journal of Adolescent and Youth Psychological Studies (JAYPS), 4(2), 86-96. https://doi.org/10.61838/kman.jayps.4.2.10
Rezapour, Y., Rabaniayn, H., & Aminjafari, F. (2025). The Mediating Role of Cognitive Emotion Regulation in the Relationship between Attachment Styles and Attitudes Towards Marriage. Journal of Culture of Counseling and Psychotherapy, 16(61), 33-66. https://qccpc.atu.ac.ir/article_18877_en.html
Rotaru, I. C. (2019). The school dropout of Roma children. Between anti-gypsism andthe socio - economic dysfunction of Romanian educational system. International Conference “Supervision in Psycotherapy”. https://www.researchgate.net/publication/335293496_The_school_dropout_of_Roma_children_Between_anti-gypsism_and_the_socio_-economic_dysfunction_of_Romanian_educational_system
Schaap, G. M., Chakhssi, F., & Westerhof, G. J. (2016). Inpatient schema therapy for nonresponsive patients with personality pathology: Changes in symptomatic distress, schemas, schema modes, coping styles, experienced parenting styles, and mental well-being. Psychotherapy, 53(4), 402-412. https://doi.org/10.1037/pst0000056
Simmonds-Buckley, M., Osivwemu, E.-O., Kellett, S., & Taylor, C. (2022). The acceptability of cognitive analytic therapy (CAT): Meta-analysis and benchmarking of treatment refusal and treatment dropout rates. Clinical psychology review, 96(1), 102187-102197. https://doi.org/10.1016/j.cpr.2022.102187
Stratton, N., Mendoza Alvarez, M., Labrish, C., Barnhart, R., & McMain, S. (2020). Predictors of dropout from a 20-week dialectical behavior therapy skills group for suicidal behaviors and borderline personality disorder. Journal of personality disorders, 34(2), 216-230. https://doi.org/10.1521/pedi_2018_32_391
Strauss, C., Bibby-Jones, A.-M., Jones, F., Byford, S., Heslin, M., Parry, G., Barkham, M., Lea, L., Crane, R., de Visser, R., Arbon, A., Rosten, C., & Cavanagh, K. (2023). Clinical Effectiveness and Cost-Effectiveness of Supported Mindfulness-Based Cognitive Therapy Self-help Compared With Supported Cognitive Behavioral Therapy Self-help for Adults Experiencing Depression: The Low-Intensity Guided Help Through Mindfulness (LIGHTMind) Randomized Clinical Trial. JAMA Psychiatry, 80(5), 415-424. https://doi.org/10.1001/jamapsychiatry.2023.0222