Detecting Post-Traumatic Stress Risk via ML Analysis of Dissociative Tendencies and Arousal Dysregulation
Keywords:
Post-Traumatic , Stress Disorder, Machine Learning, Dissociation, Arousal DysregulationAbstract
Objective: To evaluate the predictive utility of machine learning models in detecting post-traumatic stress risk by analyzing the complex interplay between dissociative tendencies and physiological arousal markers.
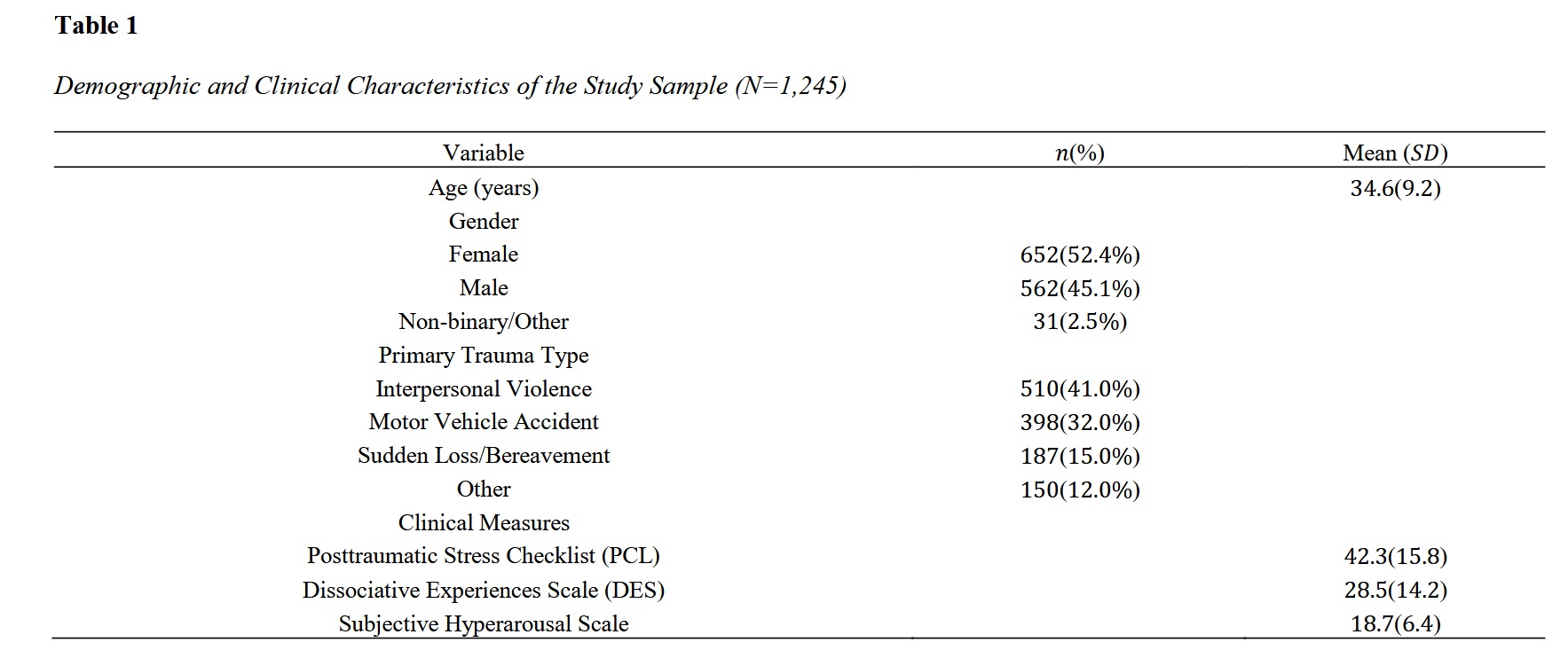
Methods and Materials: A cross-sectional observational study was conducted with a sample of N=1,245 adult participants from the USA with documented trauma exposure. Data collection utilized the Posttraumatic Stress Disorder Checklist (PCL), the Dissociative Experiences Scale (DES), subjective hyperarousal scales, and wearable biometric sensors capturing electrodermal activity and heart rate variability during a standardized stress-reactivity paradigm. Extreme Gradient Boosting, Random Forest, and Support Vector Machine algorithms were trained and evaluated using stratified ten-fold cross-validation.
Findings: The Extreme Gradient Boosting model demonstrated superior predictive performance, achieving an AUC=0.91, which significantly outperformed the Random Forest (AUC=0.88) and Support Vector Machine (AUC=0.82) models. Feature importance analysis revealed that derealization (22.4%), depersonalization (18.1%), and low heart rate variability during recovery (15.3%) were the most critical predictors of post-traumatic stress risk. Furthermore, a significant non-linear interaction demonstrated that objective physiological arousal strongly predicted risk primarily in highly dissociative individuals who underreported subjective distress.
Conclusion: Machine learning models integrating objective physiological data with subjective dissociative measures offer a powerful, highly sensitive approach for detecting hidden post-traumatic stress risk.
Downloads
References
Akay, G., Koç, E. S., & Oğuzhan, H. (2026). Examination of Post-Traumatic Stress Reaction, Quality of Life, and Loneliness Levels in Adolescents Who Experienced an Earthquake. Journal of Child & Adolescent Trauma, 1-9. https://doi.org/10.1007/s40653-026-00822-5
Atarod, N., Borjali, A., Sohrabi, F., & Basharpoor, S. (2016). The Effectiveness of Holographic Reprocessing Therapy on Arousal and Re-Experiencing Symptoms in Veterans with Post-Traumatic Stress Disorder. Urmia Medical Journal, 27(5), 427-437. https://umj.umsu.ac.ir/article-1-3556-fa.html
Boelen, P. A., van de Schoot, R., van den Hout, M. A., de Keijser, J., & van den Bout, J. (2010). Prolonged Grief Disorder, depression, and posttraumatic stress disorder are distinguishable syndromes. Journal of affective disorders, 125(1), 374-378. https://doi.org/10.1016/j.jad.2010.01.076
Danböck, S. K. (2023). Psychometric Properties of the Dissociative Subtype of Posttraumatic Stress Disorder Scale: Replication and Extension in Two German-Speaking Samples. European Journal of Psychotraumatology, 14(2). https://doi.org/10.1080/20008066.2023.2238492
Dimitrova, L. I., Fernando, V., Vissia, E. M., Nijenhuis, E. R. S., Draijer, N., & Antje, A. T. S. R. (2020). Sleep, Trauma, Fantasy and Cognition in Dissociative Identity Disorder, Post-Traumatic Stress Disorder and Healthy Controls: A Replication and Extension Study. European Journal of Psychotraumatology, 11(1). https://doi.org/10.1080/20008198.2019.1705599
Hamer, R., Bestel, N., & Mackelprang, J. L. (2024). Dissociative symptoms in complex posttraumatic stress disorder: A systematic review. Journal of Trauma & Dissociation, 25(2), 232-247. https://doi.org/10.1080/15299732.2023.2293785
Jozan, A., Fardin, M., & Sanaguye Moharer, G. (2021). The Effectiveness of Teaching Coping Skills in Posttraumatic Stress Effects’ Reductions amongst Adolescents Recovered from Corona Pandemic. Applied Family Therapy Journal (AFTJ), 2(5), 275-286. https://journals.kmanpub.com/index.php/aftj/article/view/859
McNally, R. J. (2013). Posttraumatic stress disorder and dissociative disorders. In P. H. Blaney, T. Millon, & R. F. Krueger (Eds.), Oxford Textbook of Psychopathology. Oxford University Press. https://psycnet.apa.org/record/2014-35517-007
Muhammad, S., & Abdullahi, T. (2025). Post-Traumatic Stress and Academic Adjustment Among Children Affected by Insecurity in Northern Nigeria: Strategies for Psychosocial Intervention in Schools. Federal University Gusau faculty of Education Journal, 5(4), 81-88. https://doi.org/10.64348/zije.202592
Ouimette, P., Read, J., & Brown, P. J. (2005). Consistency of retrospective reports of DSM-IV Criterion A traumatic stressors among substance use disorder patients. Journal of Traumatic Stress, 18(1), 43-51. https://doi.org/10.1002/jts.20009
Perlick, D. A., Sautter, Frederic J, ecker-Cretu, Julia J, Schultz, Danielle, Grier, Savannah C, Libin, Alexander V, Schladen, Manon Maitland, Glynn, Shirley M. (2017). The incorporation of emotion-regulation skills into couple- and family-based treatments for post-traumatic stress disorder. Military Medical Research, 4(1), 21. https://doi.org/10.1186/s40779-017-0130-9
Ratcliff, J. J., Miller, A. K., Monheim, C. L., & Rice, C. J. (2025). Posttraumatic Growth and Meaning in Life Mediate the Relationship Between Severity of Adolescent Bullying Victimization and Adulthood Health Outcomes. Journal of interpersonal violence. https://doi.org/10.1177/08862605251343203
Read, J. P., Colder, C. R., Merrill, J. E., Ouimette, P., White, J., & Swartout, A. (2012). Trauma and posttraumatic stress symptoms predict alcohol and other drug consequence trajectories in the first year of college. Journal of consulting and clinical psychology, 80(3), 426-439. https://doi.org/10.1037/a0028210
Sadeghi, K., Goodarzi, G., & Foroughi, A. (2023). Recovering from Post-Traumatic Stress Disorder symptoms: A study on the combination of art and mindfulness. Shenakht, 9(6), 131-145. https://doi.org/10.32598/shenakht.9.6.131
Sheikh, W. G. E., Abou‐Abbass, H., Bizri, M., Tamim, H., Karout, L., Allouch, F., Chehade, R., Ghannam, M., Fares, Y., Nasser, Z., Al‐Hajj, S., Harati, H., & Kobeissy, F. (2025). The Impact of Posttraumatic Stress Disorder and Head Injury on Reactive and Appetitive Aggression in Adult Syrian Refugees in Lebanon. Psychological Trauma Theory Research Practice and Policy, 17(1), 67-76. https://doi.org/10.1037/tra0001796
Trivedi, G. Y., & Thakore, P. (2025). A Case Study on Post-Traumatic Stress Disorder, Prolonged Grief Disorder, and Adjustment Disorder. Cureus. https://doi.org/10.7759/cureus.80595
Vadakkedath, R., & Thomas, S. S. (2025). Post-Traumatic Stress Disorder Among ICU Survivors. Rguhs Journal of Nursing Sciences, 15(1). https://doi.org/10.26463/rjns.15_1_15
Veronese, G., Mahamid, F., & Bdier, D. (2025). Traumatic Grief, Health and Mental Health in Palestine: The Mediating Role of Posttraumatic Growth and Resilience. Health Psychology Report. https://doi.org/10.5114/hpr/199540
Watts, J. R., Lazzareschi, N. R., Warwick, L. A., & Gaa, M. (2025). Posttraumatic stress disorder symptoms in postsecondary students exposed to childhood psychological abuse: Exploring the role of negative meta‐emotions. Journal of Counseling & Development, 103(1), 3-14. https://doi.org/10.1002/jcad.12534
Ye, T., Huang, Y., Chen, Y., Ni, Y., Zhang, X., Song, B., Lan, J., Feng, L., Liao, C., & Zheng, Y. (2025). The Mediating Role of Death Coping Between Moral Resilience and Vicarious Posttraumatic Growth Among ICU Nurses. Journal of Advanced Nursing. https://doi.org/10.1111/jan.70249
Ye, Y., Xie, Q., Sun, Y., Xu, J., Cheng, L., & Kong, L. (2025). Effects of Interpersonal Relationships and Forgiveness on Post-Traumatic Growth in Hemodialysis Patients: A Cross-Sectional Study. BMC Nephrology, 26(1). https://doi.org/10.1186/s12882-025-04141-z
Zhang, L., Wu, X., Liu, M., & Liu, A. (2025). Relationship Between Complex Posttraumatic Stress Disorder Symptoms and Posttraumatic Growth Among Adolescents and Emerging Adults With Adverse Childhood Experiences. Psychological Trauma Theory Research Practice and Policy. https://doi.org/10.1037/tra0001932
Zhao, S. (2025). Relationship Between Purposeful Rumination and Post-Traumatic Growth of College Students Who Experienced Childhood Trauma: A Regulated Intermediary Model. https://doi.org/10.20944/preprints202501.1481.v1