Explainable AI Models for Identifying Personality-Driven Risk Factors in Psychosomatic Disorders
Keywords:
Psychosomatic disorders, personality traits, explainable artificial intelligence, stress reactivity, emotional regulation, machine learningAbstract
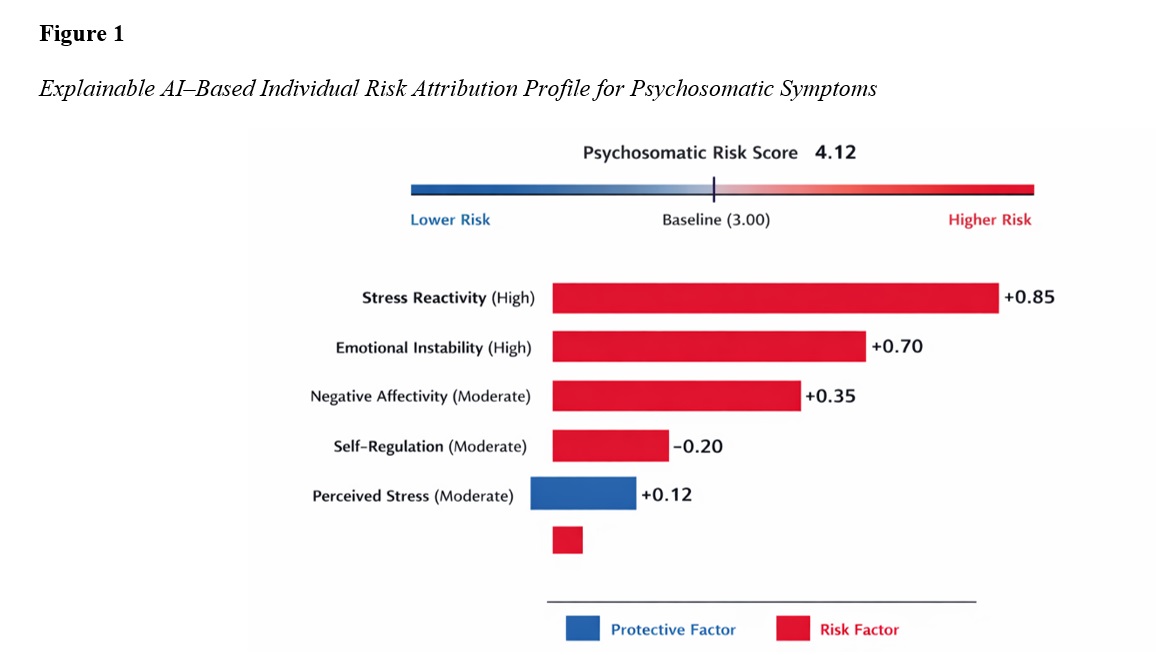
The objective of this study was to identify and transparently explain personality-driven risk factors associated with psychosomatic symptom severity using explainable artificial intelligence models. This cross-sectional study was conducted on an adult clinical sample recruited from psychosomatic and general health settings in Chile. Participants completed validated self-report instruments assessing personality traits, stress-related psychological variables, and psychosomatic symptom severity. After data preprocessing and standardization, multiple supervised machine learning models were developed to predict psychosomatic symptom severity based on personality and psychological predictors. Model performance was evaluated using cross-validation procedures. The best-performing model was further analyzed using explainable artificial intelligence techniques to identify global and individual-level contributions of predictors, enabling transparent interpretation of nonlinear effects and interactions among personality traits. Nonlinear ensemble models significantly outperformed linear models in predicting psychosomatic symptom severity, explaining a substantial proportion of variance. Stress reactivity emerged as the strongest predictor, followed by emotional instability, perceived stress, and negative affectivity. Explainable analyses revealed threshold and interaction effects, indicating sharp increases in psychosomatic risk at high levels of stress reactivity and compounded effects when combined with emotional instability. Self-regulation-related traits demonstrated a protective effect, particularly at low to moderate stress levels, although this effect diminished under extreme stress conditions. Individual-level explanations highlighted marked heterogeneity in risk profiles, with distinct personality configurations driving symptom severity across participants. The findings indicate that psychosomatic symptom severity is shaped by dynamic, nonlinear interactions among personality traits and stress-related factors rather than isolated linear effects.
Downloads
References
An, B., Sorokin, S. A., Болгов, М. И., & Smolnikova, A. O. (2023). The Impact of Depression Symptoms on Postmorbid Adaptation of Patients Who Have Undergone SARS-CoV-2 Infection (Assessment From the Position of the Multimorbidity Model). Zhurnal Nevrologii I Psikhiatrii Im S S Korsakova, 123(3), 70. https://doi.org/10.17116/jnevro202312303170
Basińska, M. A., & Woźniewicz, A. (2021). Diagnostic Criteria for Psychosomatic Research – Revised Version by Giovanni A. Fava and His Research Team. Psychiatria I Psychologia Kliniczna, 21(2), 121-127. https://doi.org/10.15557/pipk.2021.0013
Brüne, M. (2021). Mental Health and Biological Evolution: Implications for Psychiatry and Psychosomatic Medicine. Neuroforum, 0(0). https://doi.org/10.1515/nf-2020-0033
Camacho-Zamora, A., Camberos-Barraza, J., Rábago-Monzón, Á. R., Sosa-Arámbula, H. J., & Alberto, K. D. l. H.-A. (2024). Psychosomatic Influences on Insomnia: Mechanisms, Diagnosis, and Treatment Strategies. Journal of Clinical and Basic Psychosomatics, 3(1), 32. https://doi.org/10.36922/jcbp.4588
Cozzi, G., Lucarelli, A., Borrometi, F., Corsini, I., Passone, E., Pusceddu, S., Morabito, G., Barbi, E., & Benini, F. (2021). How to Recognize and Manage Psychosomatic Pain in the Pediatric Emergency Department. Italian Journal of Pediatrics, 47(1). https://doi.org/10.1186/s13052-021-01029-0
Doering, S., Herpertz, S., Pape, M., Hofmann, T., Rose, M., Imbierowicz, K., Geiser, F., Bierling, A. L., Weidner, K., Rademacher, J., Michalek, S., Morawa, E., Erim, Y., Teigelack, P., Teufel, M., Hartmann, A., Lahmann, C., Peters, E. M., Kruse, J., . . . Kessler, H. (2023). The Multicenter Effectiveness Study of Inpatient and Day Hospital Treatment in Departments of Psychosomatic Medicine and Psychotherapy in Germany. Frontiers in Psychiatry, 14. https://doi.org/10.3389/fpsyt.2023.1155582
Dolynnyi, S. (2021). Psychosomatic Factors in the Aspect of the Conflict-Generated Behaviour Development. Psychological Journal, 7(5), 50-59. https://doi.org/10.31108/1.2021.7.5.5
Dorozhenok, I. Y., Snarskaya, E. S., & Михайлова, М. В. (2021). Lichen Planus and Itch-Related Psychosomatic Disorders. Russian Journal of Skin and Venereal Diseases, 24(6), 543-551. https://doi.org/10.17816/dv100612
Evert, L., Grishkevich, N. Y., Kostyuchenko, Y., & Bakhshieva, S. A. (2023). Indicators of the Psycho-Emotional Status of Adolescents Khakassia With Different Online Behavior. V M Bekhterev Review of Psychiatry and Medical Psychology, 57(1), 71-82. https://doi.org/10.31363/2313-7053-2023-635
Fedorchuk, M. (2024). The Interaction Between Psychological Factors and Thyroid Disorders: A Psychosomatic Aspect. Kyiv Journal of Modern Psychology and Psychotherapy, 8, 147-161. https://doi.org/10.48020/mppj.2024.02.11
Huang, W. J. (2025). 252. Are Persistent Somatic Symptoms a Trans-Diagnostic Concept? A Cluster Analysis. The International Journal of Neuropsychopharmacology, 28(Supplement_2), ii103-ii103. https://doi.org/10.1093/ijnp/pyaf052.204
IuF, A. (2022). Psychogenic Depression in Pediatric Practice. Pediatria Journal Named After G N Speransky, 101(6), 146-152. https://doi.org/10.24110/0031-403x-2022-101-6-146-152
Khrol, N. V. (2024). Evolution of Understanding Psychosomatic Disorders in Medical Psychology. Psychiatry Neurology and Medical Psychology(26), 476-481. https://doi.org/10.26565/2312-5675-2024-26-11
Kirillov, I. (2023). Evaluation Criteria for Psychosomatic Practice. The Global Psychotherapist, 3(2), 57-69. https://doi.org/10.52982/lkj199
Philippova, A., Malkina, O. L., Korotun, V. L., & Shatova, E. (2023). The Role of Somatic Factors in Early Childhood and Adolescent Psychosomatic Disorders. Bangladesh Journal of Medical Science, 22(3), 687-694. https://doi.org/10.3329/bjms.v22i3.66964
Reininger, K. M., Biel, H. M., Hennig, T., Zitzmann, S., Weigel, A., Spitzer, C., Toussaint, A., & Löwe, B. (2023). Beliefs About Emotions Predict Psychological Stress Related to Somatic Symptoms. British Journal of Clinical Psychology, 62(4), 699-716. https://doi.org/10.1111/bjc.12438
Rozina, I. V. (2020). Special Features of Designing a Correction Program for Adolescents Who Have Signs of Psychosomatic Disorders. European Humanities Studies State and Society(3(II)), 19-38. https://doi.org/10.38014/ehs-ss.2020.3-2.02
Si, O., Troshina, D. V., Sokolova, P. S., & Volel, B. A. (2023). Psychosomatic Functional Disorders in Pulmonary Practice. Pulmonologiya, 33(3), 386-392. https://doi.org/10.18093/0869-0189-2023-33-3-386-392
Sukiasyan, S. G. (2021). Traditional Concepts and Approaches in Psychiatry as Preconditions for Psychosomatic Concept: Clinical and Psychopathological Aspect / Традиционные Взгляды И Походы В Психиатрии Как Предпосылки Психосоматической Концепции: Клинико-Психопатологический Аспект. Armenian Journal of Mental Health, 18-28. https://doi.org/10.55436/1829202x-12.2021.2-18
Tolokonin, A. O. (2023). Models of Pathogenesis of Psychosomatic Disorders and the Concept of Psychosomatic Scenario. Medical Herald of the South of Russia, 14(2), 61-66. https://doi.org/10.21886/2219-8075-2023-14-2-61-66
Werner, F., Schumacher, F., Mühle, C., Adler, W., Schug, C., Schäflein, E., Morawa, E., Kleuser, B., Kornhuber, J., Erim, Y., & Rhein, C. (2025). Psychosomatic - Psychotherapeutic Treatment of Stress-Related Disorders Impacts the Sphingolipid Metabolism Towards Increased Sphingosine and Sphingosine-1-Phosphate Levels. European Archives of Psychiatry and Clinical Neuroscience. https://doi.org/10.1007/s00406-025-01985-2
Xu, W., Jiang, W., Jiang, C., Sun, T., Chen, G., You, L., Cosci, F., Li, L., & Yuan, Y. (2025). Psychosomatic Symptoms in Type 2 Diabetes Patients: A Network Analysis. The International Journal of Neuropsychopharmacology, 28(Supplement_1), i56-i56. https://doi.org/10.1093/ijnp/pyae059.097
Yagudin, D. R. (2025). Neurointuitive Intelligence in Neurotherapeutic Practice: Meaning, Essence, Interrelationship. Scientific Research and Development Socio-Humanitarian Research and Technology, 14(3), 36-40. https://doi.org/10.12737/2306-1731-2025-14-3-36-40
Yi, S., Hu, X., Wang, C. C., Ge, J., Ma, Z., & Zhao, Y. (2024). Psychosomatic Health Status and Corresponding Comorbid Network Analysis of College Students in Traditional Chinese Medicine Schools. Frontiers in Psychiatry, 15. https://doi.org/10.3389/fpsyt.2024.1467064
Zimоglyad, O. E., Ivanova, Y. S., Смирнова, А. П., & Volkova, E. (2023). Alexithymia and Related Mental and Psychosomatic Disorders. Clinical Medicine (Russian Journal), 101(4-5), 223-228. https://doi.org/10.30629/0023-2149-2023-101-4-5-223-228