Neurobiological Correlates of Personality-Driven Psychosomatic Reactivity: A Psychoneuroimmunological Perspective
Keywords:
psychosomatic reactivity, personality traits, psychoneuroimmunology, cortisol, inflammationAbstract
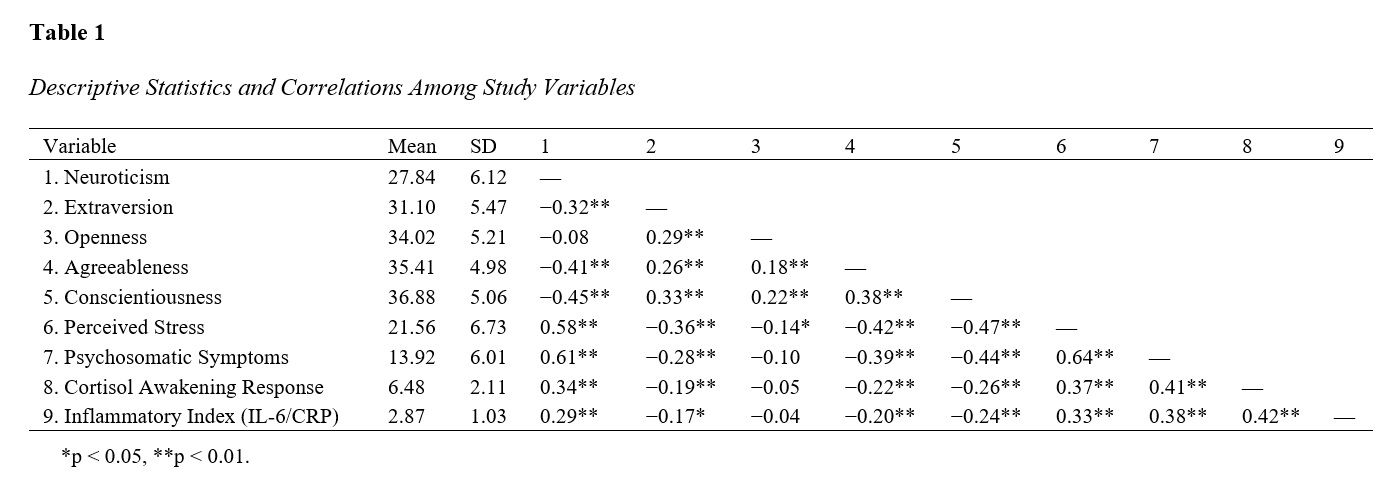
This study aimed to examine an integrated psychoneuroimmunological model linking personality traits to psychosomatic reactivity through perceived stress, neuroendocrine activity, and immune activation. A cross-sectional correlational design was employed with a community-based adult sample recruited from urban health centers in Mexico. Participants completed validated self-report measures assessing personality traits, perceived stress, and psychosomatic symptoms. Neuroendocrine activity was indexed using salivary cortisol collected at awakening and 30 minutes post-awakening, while immune activation was assessed through serum inflammatory markers, including interleukin-6 and C-reactive protein. Data were analyzed using correlation analyses, multiple regression models, mediation analyses with bootstrapping, and structural equation modeling to test direct and indirect pathways among psychological and biological variables. Inferential analyses indicated that neuroticism was a strong positive predictor of psychosomatic symptoms, whereas conscientiousness and agreeableness were significant negative predictors. Perceived stress significantly mediated the relationship between neuroticism and psychosomatic symptom severity. Elevated cortisol awakening response was associated with higher perceived stress and greater somatic symptom burden and functioned as an additional mediator. Inflammatory markers were positively associated with cortisol activity and psychosomatic symptoms. Structural equation modeling demonstrated good model fit and supported a sequential pathway from personality traits to stress appraisal, neuroendocrine dysregulation, immune activation, and psychosomatic reactivity, with protective traits exerting indirect buffering effects through reduced stress responses. The findings support a psychoneuroimmunological model in which personality traits function as central regulators of psychosomatic reactivity by shaping psychological stress appraisal and downstream neuroendocrine and immune processes, highlighting the importance of integrative, personality-informed approaches to psychosomatic health.
Downloads
References
BaŞ, F. Y., Temel, E. N., & Çankaya, B. A. (2021). The Associ̇ati̇on of Type D Personali̇ty and Premenstruel Syndrome. https://doi.org/10.22541/au.162648142.21206034/v1
Bendezú, J. J., Calhoun, C. D., Vinograd, M., Patterson, M. W., Rudolph, K. D., Giletta, M., Hastings, P. D., Nock, M. K., Slavich, G. M., & Prinstein, M. J. (2022). Exploring Joint HPA–inflammatory Stress Response Profiles in Adolescent Girls: Implications for Developmental Models of Neuroendocrine Dysregulation. Developmental Psychobiology, 64(3). https://doi.org/10.1002/dev.22247
Chen, S. J., Chang, H. C., & Gau, S. Y. (2025). Psoriasis Patients Are Associated With Increased Risk of New-Onset Irritable Bowel Syndrome: A Multicenter, Retrospective Cohort Study. International Journal of Medical Sciences, 22(13), 3422-3428. https://doi.org/10.7150/ijms.116551
Császár-Nagy, N., & Bókkon, I. (2023). Hypnotherapy and IBS: Implicit, Long-Term Stress Memory in the ENS? Heliyon, 9(1), e12751. https://doi.org/10.1016/j.heliyon.2022.e12751
Czerwińska, K., Gać, P., Poręba, R., Mazur, G., & Pawlas, K. (2021). Cardiac and Vascular Disorders as Para-Occupational Diseases – A Polish Perspective. Annals of Agricultural and Environmental Medicine, 28(2), 231-236. https://doi.org/10.26444/aaem/122259
Dattolo, A., Tan, I. J., & Jafferany, M. (2025). Psychoanalytic and Psychodynamic Approaches to Skin Disease and Their Implications for Dermatology. Skin Research and Technology, 31(2-5). https://doi.org/10.1111/srt.70176
Gano, A., Barney, T. M., Vore, A. S., Mondello, J. E., Varlinskaya, E. I., Pautassi, R. M., & Deak, T. (2023). Cues Associated With a Single Ethanol Exposure Elicit Conditioned Corticosterone Responses in Adolescent Male but Not Female Sprague–Dawley Rats. Developmental Psychobiology, 66(1). https://doi.org/10.1002/dev.22442
Hasanah, I., Nursalam, N., Haikal, Z., Azizah, A. M., & Rohita, T. (2023). Impact of IV-line Insertion on Salivary Cortisol Levels as a Stress Biomarker in Children. Open Access Macedonian Journal of Medical Sciences, 11(B), 60-64. https://doi.org/10.3889/oamjms.2023.10268
Jafferany, M., Ferreira, B. R., Abdelmaksoud, A., & Mkhoyan, R. (2020). Management of Psychocutaneous Disorders: A Practical Approach for Dermatologists. Dermatologic Therapy, 33(6). https://doi.org/10.1111/dth.13969
Jiang, Z., Lin, G., Chen, J., Chen, J., Jiang, H., Feng, L., Jiang, X., Jin, M., Lou, J., & Ni, Z. (2021). The Influence of Personality Traits on Mental Symptoms in 5, 449 Chinese University Volunteers: A Cross-Sectional Study. SSRN Electronic Journal. https://doi.org/10.2139/ssrn.3848525
Kim, Y., Jung, Y., Kang, I., & Yeo, E. J. (2025). Understanding Sex Differences in Autoimmune Diseases: Immunologic Mechanisms. International Journal of Molecular Sciences, 26(15), 7101. https://doi.org/10.3390/ijms26157101
Kolniak‐Ostek, J. (2025). Fermented Means Beneficial – Fermented Foods as Support for the Metabolism Of children and Adolescents? Pediatric Endocrinology Diabetes and Metabolism, 31(2), 41-43. https://doi.org/10.5114/pedm.2025.152593
Lages, Y., & McNaughton, N. (2022). Non-Human Contributions to Personality Neuroscience – From Fish Through Primates. An Introduction to the Special Issue. Personality neuroscience, 5. https://doi.org/10.1017/pen.2022.4
Latifi, A., & Flegr, J. (2025). Beyond Latency: Chronic Toxoplasma Infection and Its Unveiled Behavioral and Clinical Manifestations—A 30-Year Research Perspective. Biomedicines, 13(7), 1731. https://doi.org/10.3390/biomedicines13071731
Liu, S., Cheng, L., Liu, Y., Zhan, S., Wu, Z., & Zhang, X. (2023). Relationship Between Dietary Polyphenols and Gut Microbiota: New Clues to Improve Cognitive Disorders, Mood Disorders and Circadian Rhythms. Foods, 12(6), 1309. https://doi.org/10.3390/foods12061309
Mahony, C., & Ryan, C. O. (2022). A Molecular Framework for Autistic Experiences: Mitochondrial Allostatic Load as a Mediator Between Autism and Psychopathology. https://doi.org/10.20944/preprints202205.0281.v1
Millet, A., & Jendzjowsky, N. (2023). Pathogen Recognition by Sensory Neurons: Hypotheses on the Specificity of Sensory Neuron Signaling. Frontiers in Immunology, 14. https://doi.org/10.3389/fimmu.2023.1184000
Rajeev, A., Sudheer, A., & Chattopadhyay, I. (2024). Probiotics as a Sustainable Approach in Health Enrichment. Journal of Pure and Applied Microbiology, 18(1), 80-99. https://doi.org/10.22207/jpam.18.1.02
Rovnaghi, C. R., Rigdon, J., Roué, J. M., Ruiz, M. O., Carrión, V. G., & Anand, K. J. S. (2021). Longitudinal Trajectories of Hair Cortisol: Hypothalamic-Pituitary-Adrenal Axis Dysfunction in Early Childhood. Frontiers in Pediatrics, 9. https://doi.org/10.3389/fped.2021.740343
Salberg, S., Sgro, M., Brady, R. D., Noel, M., & Mychasiuk, R. (2020). The Development of Adolescent Chronic Pain Following Traumatic Brain Injury and Surgery: The Role of Diet and Early Life Stress. Developmental Neuroscience, 42(1), 2-11. https://doi.org/10.1159/000508663
Scarola, S., & Bardi, M. (2020). Environmental Enrichment Modulates Inflammation During Development in Long‐evans Rats (Rattus Norvegicus). Developmental Psychobiology, 63(2), 183-191. https://doi.org/10.1002/dev.22007
Tian, R.-N. (2025). Association Between the Dietary Inflammatory Index and Depressive Symptoms in Adults With Cardiovascular–kidney–metabolic Syndrome: Evidence of Metabolic Syndrome as a Mediator. Frontiers in Nutrition, 12. https://doi.org/10.3389/fnut.2025.1623482
Tidmarsh, L. V., Harrison, R., Ravindran, D., Matthews, S. L., & Finlay, K. A. (2022). The Influence of Adverse Childhood Experiences in Pain Management: Mechanisms, Processes, and Trauma-Informed Care. Frontiers in Pain Research, 3. https://doi.org/10.3389/fpain.2022.923866
Troubat, R., Barone, P., Leman, S., Desmidt, T., Cressant, A., Atanasova, B., Brizard, B., El‐Hage, W., Surget, A., Belzung, C., & Camus, V. (2020). Neuroinflammation and Depression: A Review. European Journal of Neuroscience, 53(1), 151-171. https://doi.org/10.1111/ejn.14720
Vassiliadi, D. A., Vassiliou, A. G., Ilias, Ι., Tsagarakis, S., Kotanidou, Α., & Dimopoulou, I. (2021). Pituitary–Adrenal Responses and Glucocorticoid Receptor Expression in Critically Ill Patients With COVID-19. International Journal of Molecular Sciences, 22(21), 11473. https://doi.org/10.3390/ijms222111473
Vlachos, I. I., Papageorgiou, C., & Margariti, M. (2020). Neurobiological Trajectories Involving Social Isolation in PTSD: A Systematic Review. Brain Sciences, 10(3), 173. https://doi.org/10.3390/brainsci10030173
Wang, S., Luo, J., Wang, H., Chen, T., Sun, J., Xi, Q., & Zhang, Y. (2024). Extracellular Vesicles: A Crucial Player in the Intestinal Microenvironment and Beyond. International Journal of Molecular Sciences, 25(6), 3478. https://doi.org/10.3390/ijms25063478
Wang, Z., Wang, X., Li, Y., Zhao, Q., Lan, Z., & Li, W. (2025). Integrated Multi-Omics Analysis Reveals Immune and Metabolic Dysregulation in a Restraint Stress-Induced Depression Model. Biomedicines, 13(9), 2183. https://doi.org/10.3390/biomedicines13092183
Whiston, A., Igou, E. R., Fortune, D. G., Team, A. D., & Semkovska, M. (2023). Examining Stress and Residual Symptoms in Remitted and Partially Remitted Depression Using a Wearable Electrodermal Activity Device: A Pilot Study. Ieee Journal of Translational Engineering in Health and Medicine, 11, 96-106. https://doi.org/10.1109/jtehm.2022.3228483
Zhao, X., Li, H., & Dai, R. P. (2022). Neuroimmune Crosstalk Through Brain-Derived Neurotrophic Factor and Its Precursor Pro-Bdnf: New Insights Into Mood Disorders. World journal of psychiatry, 12(3), 379-392. https://doi.org/10.5498/wjp.v12.i3.379