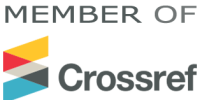Modeling Personality–Emotion–Somatic Symptom Pathways with Explainable Machine Learning
Keywords:
Somatic symptoms, personality traits, neuroticism, emotional distress, explainable machine learning, SHAP, psychosomatic healthAbstract
This study aimed to examine the pathways linking personality traits, emotional distress, and somatic symptoms using explainable machine learning techniques. This cross‑sectional study included 1,024 adults from Mexico (54.3% women; mean age = 34.7 years, SD = 11.2). Participants completed validated psychological instruments, including the Big Five Inventory (BFI‑44) to assess personality traits, the Depression Anxiety Stress Scales (DASS‑21) to measure emotional distress, and the Patient Health Questionnaire Somatic Symptom Scale (PHQ‑15) to assess somatic symptom severity. Descriptive statistics and Pearson correlations were first conducted to examine relationships among variables. Subsequently, machine learning models—Random Forest, Gradient Boosting, and XGBoost—were developed to predict somatic symptoms. Model performance was evaluated using the coefficient of determination (R²), and SHapley Additive exPlanations (SHAP) were used to identify the relative importance of predictors and interpret the models. Correlation analyses indicated significant positive associations between neuroticism, depression, anxiety, stress, and somatic symptoms (r range = .29–.48, p < .001). Neuroticism showed the strongest correlations with anxiety (r = .48) and somatic symptoms (r = .41). Among the machine learning models, XGBoost demonstrated the best predictive performance (R² = 0.42), followed by Gradient Boosting (R² = 0.39) and Random Forest (R² = 0.36). SHAP analyses revealed that anxiety and neuroticism were the most influential predictors of somatic symptoms, followed by stress and depression. Interaction analysis suggested that individuals with high neuroticism combined with high anxiety exhibited nearly twice the predicted level of somatic symptom severity compared to individuals with low scores on these variables. The findings highlight the central role of emotional distress and neuroticism in predicting somatic symptoms and demonstrate the value of explainable machine learning for identifying complex psychosomatic pathways.
Downloads
References
Allemand, M., Fend, H., & Hill, P. L. (2024). Negative Emotional Reactivity and Somatic Symptoms During Adolescence Predict Adult Health and Wellbeing in Early and Middle Adulthood. Journal of youth and adolescence, 53(7), 1513-1528. https://doi.org/10.1007/s10964-024-01940-9
Babakhanlou, A. (2023). Presenting Structural Model of Emotional Eating in People with Obesity based on Self-Regulation with the Mediating Role of Emotional Processing. Journal of Psychological Dynamics in Mood Disorders (PDMD), 2(2), 30-40. https://doi.org/10.22034/pdmd.2023.185859
Bulut, S., Bukhori, B., & Bhat, R. H. (2024). The Experience of Psychosomatic Disorders among Adolescents: Challenges and Coping Strategies. Journal of Personality and Psychosomatic Research (JPPR), 2(2), 19-25. https://doi.org/10.61838/kman.jppr.2.2.4
Efremov, A. (2023). Eliminating Psychosomatic Pain and Negative Emotions With Dehypnosis. Journal of Organizational Behavior Research, 8(1), 1-11. https://doi.org/10.51847/rnrhuqmtqy
Erbildim, E., & Nweke, G. E. (2025). The Mediator Role of Difficulties in Emotion Regulation in the Relationship Between Guilt and Shame-Proneness and Somatic Symptoms. https://doi.org/10.21203/rs.3.rs-5930990/v1
Farahi, S., Naziri, G., Davodi, A., & Fath, N. (2023). The Mediating Role of Cognitive Emotion Regulation Strategies in the Relationship Between Early Maladaptive Schemas, Alexithymia, and Emotional Intelligence With Somatic Symptoms in People With Somatic Symptoms Disorder. Practice in Clinical Psychology, 11(3), 187-200. https://doi.org/10.32598/jpcp.11.3.887.1
Ghanavati, M. (2024). Comparing the Effectiveness of Emotion-Based and Attachment-Based Family Therapy on Emotional Distress Tolerance, Self-Differentiation and Alexithymia in Adolescent Girls With Psychosomatic Disorders. PDMD, 3(4), 139-152. https://doi.org/10.61838/kman.pdmd.3.4.10
Kang, S., Park, C. I., Kim, S. J., & Kang, J. I. (2025). Associations Between Emotional Awareness Deficits and Somatic Symptoms in a Community and Clinical Populations: A Cross-Sectional Study. BMC psychology, 13(1). https://doi.org/10.1186/s40359-025-03087-z
Lee, D., Kim, S. J., Cheon, J., Jung, Y. C., & Kang, J. I. (2024). Changes in Interoceptive Accuracy Related to Emotional Interference in Somatic Symptom Disorder. BMC psychology, 12(1). https://doi.org/10.1186/s40359-024-01778-7
Majlessi Koupaei, H., & Farista, R. (2024). Psychological Pathways to Immunity: The Role of Emotions and Stress in Health and Disease. Journal of Personality and Psychosomatic Research (JPPR), 2(1), 1-3. https://doi.org/10.61838/kman.jppr.2.1.1
Mohammadi Begi, M. (2023). A structural model predicting somatic symptoms based on childhood trauma, emotional alexithymia, and perceived social support with the mediating role of depression/anxiety/stress in patients with epilepsy
Orzechowska, A., Maruszewska, P., Gałecka, M., Hyland, P., Boduszek, D., Gałecki, P., & Bliźniewska-Kowalska, K. (2023). Emotional Control in Selected Somatic and Psychiatric Diseases. BMC psychiatry, 23(1). https://doi.org/10.1186/s12888-023-05321-7
Petzke, T. M., & Witthöft, M. (2024). The Association of Emotion Regulation and Somatic Symptoms. Psychosomatic Medicine, 86(6), 561-568. https://doi.org/10.1097/psy.0000000000001310
Saadati, N., Kiliçaslan, F., & Salami, M. O. (2024). The Psychosomatic Effects of Childhood Trauma: Insights from Adult Survivors. Journal of Personality and Psychosomatic Research (JPPR), 2(2), 34-40. https://doi.org/10.61838/kman.jppr.2.2.6
Sefotho, M. M., Serjanaj, B., Karthik, S., & Saadati, S. A. (2024). The Psychosomatic Interface of Stress and Skin Disorders: Patient Experiences and Perceptions. Journal of Personality and Psychosomatic Research (JPPR), 2(2), 26-33. https://doi.org/10.61838/kman.jppr.2.2.5
Yang, Y. (2023). A Daily Diary Study on Stressors, Hurt Feelings, Aggression, and Somatic Symptoms: The Role of Rejection Sensitivity and Negative Emotion Differentiation. Aggressive Behavior, 49(4), 371-383. https://doi.org/10.1002/ab.22076