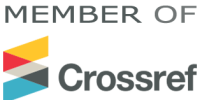Using Machine Learning to Identify Latent Profiles of Somatosensory Amplification and Catastrophic Misinterpretation of Bodily Cues in Psychosomatic Patients
Keywords:
Psychosomatic Disorders, Somatosensory Amplification, Catastrophic Misinterpretation, Latent Profile Analysis, Machine Learning, Body Sensations QuestionnaireAbstract
The study aimed to identify distinct latent profiles of psychosomatic patients based on their levels of somatosensory amplification and catastrophic misinterpretation of bodily cues using a person-centered machine learning approach. This cross-sectional study involved a sample of psychosomatic patients recruited from clinical settings in South Africa. Participants were assessed using the Somatosensory Amplification Scale (SSAS) and the Body Sensations Questionnaire (BSQ). Statistical analysis was performed using Gaussian Mixture Modeling (Latent Profile Analysis) to identify unobserved subpopulations. Model selection was determined by fit indices, including the Akaike Information Criterion (AIC), Bayesian Information Criterion (BIC), and the Lo-Mendell-Rubin Likelihood Ratio Test (LMR-LRT). A strong significant positive correlation was observed between somatosensory amplification and the catastrophic misinterpretation of bodily cues ( , ). Latent Profile Analysis identified an optimal three-profile solution: “Low Symptom Burden” ( ; ), “Moderate Symptom Burden” ( ; ), and “Severe Symptom Burden” ( ; ). Comparative analyses revealed that the “Severe Symptom Burden” profile was characterized by a significantly higher proportion of female participants, higher unemployment rates, and longer illness durations ( ), whereas age and educational background did not significantly differentiate the groups. The identification of three distinct latent profiles underscores the clinical heterogeneity of psychosomatic populations and highlights the necessity for tailored, precision-based psychological interventions that address specific levels of cognitive-perceptual distortion.
Downloads
References
Asanova, A., & Mukharovska, I. (2023). Study of Psychological Phenomena in the Structure of Chronic Pain: Depression, Anxiety, Catastrophizing. Literature Review. Psychosomatic Medicine and General Practice, 8(4). https://doi.org/10.26766/pmgp.v8i4.505
Asanova, A., Хаустова, О., Skrynnyk, O., & Mukharovska, I. (2025). Psychological, Clinical and Socio-Demographic Predictors of Pain Catastrophizing in Chronic Pain Patients: Insights From a Cross-Sectional Study. International Neurological Journal, 20(8), 411-421. https://doi.org/10.22141/2224-0713.20.8.2024.1124
Doménech, J., Angulo, A. E., Peñalver-Barrios, L., Rio-González, E. D., Herrero, R., García‐Palacios, A., Díaz, M. M., Garreta-Catalá, I., Díez-Ulloa, M.-A., & Baños-Rivera, R. M. (2025). Catastrophizing and Fear Avoidance Beliefs in Chronic Low Back Pain: A Cross-Sectional Study. European Journal of Physical and Rehabilitation Medicine, 61(2). https://doi.org/10.23736/s1973-9087.25.08419-9
Drahovzal, D. N., Stewart, S. H., & Sullivan, M. (2006). Tendency to Catastrophize Somatic Sensations: Pain Catastrophizing and Anxiety Sensitivity in Predicting Headache. Cognitive behaviour therapy, 35(4), 226-235. https://doi.org/10.1080/16506070600898397
Goodin, B. R., McGuire, L., Stapleton, L. M., Quinn, N. B., Fabian, L. A., Haythornthwaite, J. A., & Edwards, R. R. (2009). Pain Catastrophizing Mediates the Relationship Between Self-Reported Strenuous Exercise Involvement and Pain Ratings: Moderating Role of Anxiety Sensitivity. Psychosomatic Medicine, 71(9), 1018-1025. https://doi.org/10.1097/psy.0b013e3181bc62ba
Heule, M. (2025). Adverse Childhood Experiences and Urogenital Pain: Examining the Mediating Effects of Negative Affect and Pain Catastrophizing. Neurourology and Urodynamics. https://doi.org/10.1002/nau.70022
Hooshmandi, R., Aljaberi, M. A., Hammadi, F., & Ma, J. (2024). The Impact of Interoceptive Awareness on Pain Catastrophizing and Illness Perception. Journal of Personality and Psychosomatic Research (JPPR), 2(2), 4-10. https://doi.org/10.61838/kman.jppr.2.2.2
Kealy, D., Rice, S. M., Chartier, G. B., & Cox, B. J. (2021). Investigating Attachment Insecurity and Somatosensory Amplification, and the Mediating Role of Interpersonal Problems. European Journal of Health Psychology, 28(3), 120-130. https://doi.org/10.1027/2512-8442/a000078
Kearney, B. E., & Lanius, R. A. (2022). The brain-body disconnect: A somatic sensory basis for trauma-related disorders [Review]. Frontiers in Neuroscience, 16. https://doi.org/10.3389/fnins.2022.1015749
Köteles, F., & Witthöft, M. (2017). Somatosensory amplification–An old construct from a new perspective. Journal of psychosomatic research, 101, 1-9.
MacDonald, T. M., Fisk, J. D., Bernstein, C. N., El-Gabalawy, R., Hitchon, C. A., Kornelsen, J., Patten, S. B., Tisseverasinghe, A., & Marrie, R. A. (2021). The association between childhood maltreatment and pain catastrophizing in individuals with immune-mediated inflammatory diseases. Journal of psychosomatic research, 145, 110479. https://www.sciencedirect.com/science/article/pii/S0022399921001240
Moreira, M. F., & Oliveira, M. A. P. (2025). Exploring the interplay between catastrophizing and endometriosis pain through 2-wave and intensive longitudinal data. Pain Medicine, 26(4), 207-215. https://doi.org/10.1093/pm/pnae132
Nakao, M., & Takeuchi, T. (2018). Alexithymia and somatosensory amplification link perceived psychosocial stress and somatic symptoms in outpatients with psychosomatic illness. Journal of clinical medicine, 7(5), 112. https://doi.org/10.3390/jcm7050112
Ogawa, M., Saito, A., Karukivi, M., & Lahti, S. (2024). Associations of Sensory Sensitivity, Pain Catastrophizing, and Alexithymia With Dental Anxiety. European Journal of Oral Sciences, 132(2). https://doi.org/10.1111/eos.12973
Sayed Alitabar, S. H., & Goli, F. (2023). The Interplay of Neuroticism and Self-Efficacy in Pain Catastrophizing: A Quantitative Analysis. Journal of Personality and Psychosomatic Research (JPPR), 1(2), 19-24. https://doi.org/10.61838/kman.jppr.1.2.4
Stein, A., Johnson, B. N., Kelly, A. G., Cheavens, J. S., & McKernan, L. C. (2025). Negative Affect and Pain Catastrophizing Link Borderline Personality Disorder to Pain: Replicating and Extending the Borderline Personality Disorder–pain Association. Personality Disorders Theory Research and Treatment, 16(2), 173-183. https://doi.org/10.1037/per0000704
Sullivan, M. J. L., Lynch, M. E., & Clark, A. J. (2005). Dimensions of catastrophic thinking associated with pain experience and disability in patients with neuropathic pain conditions. Pain, 113(3). https://journals.lww.com/pain/fulltext/2005/02000/dimensions_of_catastrophic_thinking_associated.10.aspx
Ying Zhou, B. S. N. (2024). Relationship between pain resilience and pain catastrophizing in older patients after total knee arthroplasty: Chain-mediating effects of cognitive emotion regulation and pain management self-efficacy. Geriatric Nursing, 59, 571-580. https://doi.org/10.1016/j.gerinurse.2024.08.011