The Relationship between Self-Compassion, Interpersonal Emotion Regulation, and Coping Styles with Quality of Life in Women after Mastectomy Surgery
Keywords:
Self-compassion, Interpersonal emotion regulation, Coping styles, Quality of life, Women, Mastectomy surgeryAbstract
Objective: The aim of the present study was to examine the relationship between self-compassion, interpersonal emotion regulation, and coping styles with quality of life in women after mastectomy surgery.
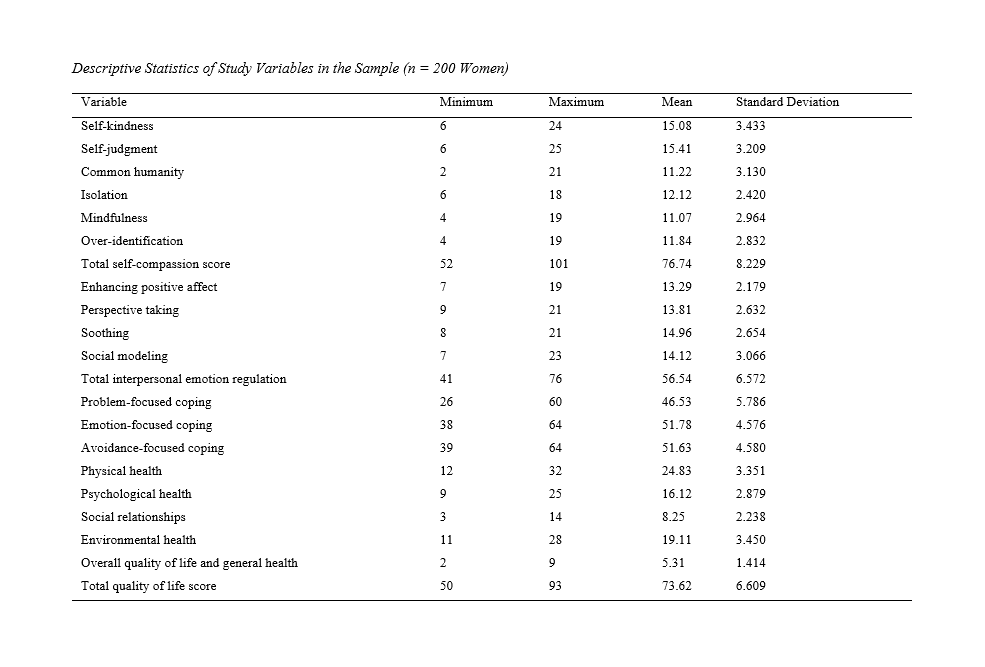
Methods and Materials: The research method was correlational, and the statistical population included women with a history of mastectomy surgery, from whom 200 participants were selected using convenience sampling. Data were collected using the Self-Compassion Scale (SCS; Neff, 2003), the Interpersonal Emotion Regulation Questionnaire (IERQ; Hofmann et al., 2016), the Coping Inventory for Stressful Situations (CISS; Parker & Endler, 1990), and the World Health Organization Quality of Life Questionnaire (WHOQOL-BREF; World Health Organization, 1991). The collected data were analyzed using Pearson correlation and multivariate regression analyses.
Findings: The results of multivariate regression analysis indicated that problem-focused coping, interpersonal emotion regulation, and self-compassion positively and significantly predicted quality of life in women after mastectomy surgery (p < .05), whereas emotion-focused coping and avoidance-focused coping negatively and significantly predicted quality of life (p < .05).
Conclusion: Higher quality of life in women after mastectomy surgery is associated with the use of problem-focused coping strategies, effective interpersonal emotion regulation, and greater self-compassion. Therefore, training in effective coping strategies for dealing with post-surgical life challenges, as well as strengthening self-compassion, should be considered by health psychology professionals to improve the quality of life of these women.
Downloads
References
Asselmann, E., Bendau, A., Hoffmann, C., & et al. (2024). Self-compassion Predicts Higher Affective Well-being and Lower Stress Symptoms Through Less Dysfunctional Coping: A Three-wave Longitudinal Study During the COVID-19 Pandemic. Journal of Happiness Studies, 25, 55. https://doi.org/10.1007/s10902-024-00755-6
Bailey, C. R., Ogbuagu, O., Baltodano, P. A., Simjee, U. F., Manahan, M. A., Cooney, D. S., & et al. (2017). Quality-of-life outcomes improve with nipple-sparing mastectomy and breast reconstruction. Plastic and Reconstructive Surgery, 140(2), 219-226. https://doi.org/10.1097/PRS.0000000000003505
Barthel, A. L., Hay, A., Doan, S. N., & Hofmann, S. G. (2018). Interpersonal emotion regulation: A review of social and developmental components. Behaviour Change, 35(4), 203-216. https://doi.org/10.1017/bec.2018.19
Bedir, M., & Eliüşük-Bülbül, A. (2024). The effect of the self-compassion program on self-compassion and professional quality of life among healthcare professionals. Current Psychology, 43(17), 15376-15384. https://doi.org/10.1007/s12144-023-05516-x
Bian, J., Chen, F., Fang, S., & Wang, Y. (2025). Self-compassion intervention programs for nurses: A scoping review. Healthcare (Basel), 13(2), 177. https://doi.org/10.3390/healthcare13020177
Carreiro, J. P., Cardoso, S., Teques, P., Teques, A. P., & Ribeiro, J. L. P. (2025). Satisfaction With Social Support and Quality of Life Among Portuguese Patients With Breast Cancer: Mediating Effects of Coping Styles—Cross-Sectional Study. Healthcare, 13(3), 297. https://doi.org/10.3390/healthcare13030297
Cho, Y. U., Lee, B. G., & Kim, S. H. (2020). Coping style at diagnosis and its association with subsequent health-related quality of life in women with breast cancer: A 3-year follow-up study. European Journal of Oncology Nursing, 45, 101726. https://doi.org/10.1016/j.ejon.2020.101726
Chukwuorji, J. C., Odi, C. P., Chike-Okoli, A., Morah, N. M., Osondu, O. M., Rukmi, D. K., Victor-Aigbodion, V., & Eze, J. E. (2024). Health-related quality of life of people living with HIV: contributions of emotion regulation and self-compassion. Venereology, 3(3), 136-146. https://doi.org/10.3390/venereology3030011
Dixon-Gordon, K. L., Bernecker, S. L., & Christensen, K. (2015). Recent innovations in the field of interpersonal emotion regulation. Current opinion in psychology, 3, 36-42. https://doi.org/10.1016/j.copsyc.2015.02.001
Dixon-Gordon, K. L., Haliczer, L. A., Conkey, L. C., & Whalen, D. J. (2018). Difficulties in interpersonal emotion regulation: Initial development and validation of a self-report measure. Journal of psychopathology and behavioral assessment, 40, 528-549. https://doi.org/10.1007/s10862-018-9647-9
Ghazafari, A., & Nikoogoftar, M. (2021). Women's Lived Experiences of Femininity after Mastectomy and Treatment: A Qualitative Study. Iranian Journal of Breast Diseases, 14(1), 36-48. https://doi.org/10.30699/ijbd.14.1.36
Gökdağ, C., Sorias, O., Kiran, S., & Sibel, G. (2019). Adaptation of the interpersonal emotion regulation questionnaire to the Turkish language and investigation of its psychometric properties. Turk Psikiyatri Dergisi, 30(1), 57. https://doi.org/10.5080/u23067
Hofmann, S. G. (2014). Interpersonal emotion regulation model of mood and anxiety disorders. Cognitive therapy and research, 38, 483-492. https://doi.org/10.1007/s10608-014-9620-1
Lee, A., Wong, Y., & Neo, X. S. (2024). Coping Mechanisms Among Patients with Terminal Illnesses. KMAN Counseling & Psychology Nexus, 2(1), 91-97. https://doi.org/10.61838/kman.psychnexus.2.1.14
Lotfi, M., Shiasy, Y., Amini, M., Mansori, K., Hamzezade, S., Salehi, A., & et al. (2020). Investigating psychometric properties of Interpersonal Emotion Regulation Questionnaire (IERQ) in university students. Journal of Mazandaran University of Medical Sciences, 30(185), 74-85. https://jmums.mazums.ac.ir/article-1-14163-en.html
Marafioti, G., Cardile, D., Culicetto, L., Quartarone, A., & Lo Buono, V. (2024). The Impact of Social Cognition Deficits on Quality of Life in Multiple Sclerosis: A Scoping Review. Brain Sciences, 14(7), 691. https://doi.org/10.3390/brainsci14070691
Martins Faria, B., Martins Rodrigues, I., Verri Marquez, L., da Silva Pires, U., & Vilges de Oliveira, S. (2021). The impact of mastectomy on body image and sexuality in women with breast cancer: a systematic review. Psicooncología, 18(1). https://psycnet.apa.org/record/2021-50274-005
Masoumi, S., Amiri, M., & Afrashteh, M. Y. (2022). Self-Compassion: The Factor That Explains a Relationship between Perceived Social Support and Emotional Self-Regulation in Psychological Well-Being of Breast Cancer Survivors. Iranian Journal of Psychiatry, 17(3), 341. https://doi.org/10.18502/ijps.v17i3.9734
Mohammadipour, M., & Pidad, F. (2021). Coping strategies, locus of control, and quality of life in patients with early-stage breast cancer. The Journal of psychology, 155(4), 375-386. https://doi.org/10.1080/00223980.2020.1816873
Moura, R., Camilo, C., & Luís, S. (2021). As strong as we are united: Effects of intrapersonal and interpersonal emotion regulation on quality of life in women with breast cancer. Frontiers in psychology, 12, 661496. https://doi.org/10.3389/fpsyg.2021.661496
Parkinson, B., & Manstead, A. S. (2015). Current emotion research in social psychology: Thinking about emotions and other people. Emotion Review, 7(4), 371-380. https://doi.org/10.1177/1754073915590624
Rashidi Mehr, F., Lashgari, M., & Abdi, H. (2023). Effectiveness of Self-compassion Training on Negative and Positive Affects, Psychological Resilience and Quality of Life of Drug Addicts. medical journal of mashhad university of medical sciences, 66(4), 993-1009. https://mjms.mums.ac.ir/article_24241.html?lang=en
Sadeghi, R., sodani, M., & gholamzadeh jofreh, M. (2020). The Effectiveness of Self-Compassion Focused Training on Reducing Negative Affect and Improving the Quality of Life in Substance-Dependent Individuals. Research on Addiction, 14(57), 131-150. https://doi.org/10.29252/etiadpajohi.14.57.131
Wild, M. G., Coppin, J. D., Mendoza, C., Metts, A., Pearson, R., & Creech, S. K. (2025). Self-compassion, mindfulness, and emotion regulation predict multiple dimensions of quality of life in US post-9/11 veterans. Quality of Life Research, 1-10. https://doi.org/10.1007/s11136-025-03908-
Wilski, M., Gabryelski, J., Brola, W., & Tomasz, T. (2019). Health-related quality of life in multiple sclerosis: Links to acceptance, coping strategies and disease severity. Disability and Health Journal, 12(4), 608-614. https://doi.org/10.1016/j.dhjo.2019.06.003
Xie, Q. (2023). Coping Style as a Mediator in the Associations Between Dispositional Mindfulness, Self-Compassion, and Loneliness. https://doi.org/10.31234/osf.io/5u7g6
Zerach, G. (2025). The Beneficial Effect of Self-Compassion on PTSD and Complex PTSD Symptoms Among Israeli Female Veterans: The Role of Coping Strategies. Psychology of Consciousness Theory Research and Practice, 12(2), 253-268. https://doi.org/10.1037/cns0000409