A Network‑Informed Machine Learning Model of How Trait Negative Affectivity and Pain Catastrophizing Predict Somatic Symptom Intensity
Keywords:
Somatic Symptom Intensity, Trait Negative Affectivity, Pain Catastrophizing, Network Analysis, Machine Learning, HelplessnessAbstract
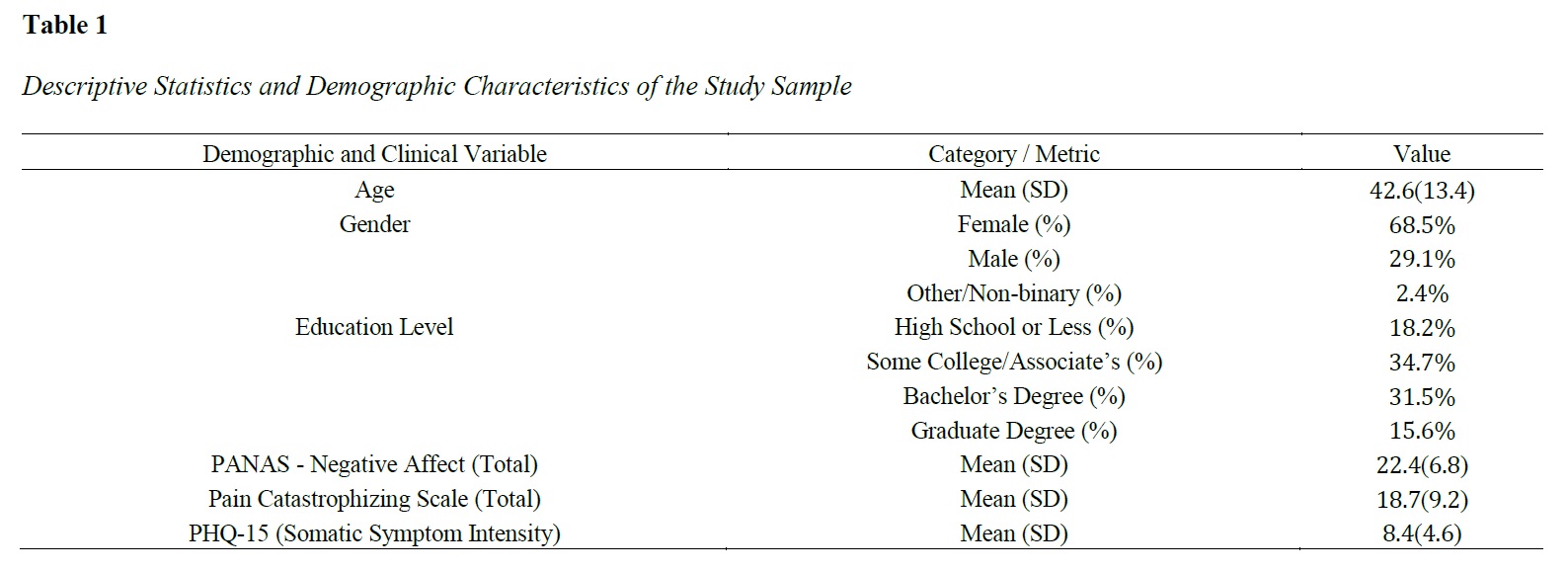
The objective of this study was to estimate a psychological network of trait negative affectivity and pain catastrophizing to identify critical bridge nodes, and subsequently utilize these specific structural bridges as features in a machine learning model to predict the continuous intensity of somatic symptoms. This cross-sectional study recruited a community sample of adults from Georgia who completed standardized online self-report questionnaires, including the Positive and Negative Affect Schedule (PANAS-NA), the Pain Catastrophizing Scale (PCS), and the Patient Health Questionnaire (PHQ-15). Data analysis utilized a two-phase methodology: first, a regularized partial correlation network analysis was conducted to map item-level interactions and compute bridge expected influence; second, machine learning algorithms (Random Forest, Support Vector Regression, Elastic Net) were trained using the identified bridge nodes as input features to predict somatic symptom intensity. Macroscopic analyses demonstrated robust positive correlations between negative affectivity, catastrophizing, and somatic burden. Network analysis revealed that the emotional state of feeling “afraid” and the cognitive appraisal of “helplessness” served as the paramount structural bridge nodes connecting the two psychological constructs. The network-informed Random Forest model demonstrated strong predictive performance on unseen test data ( ), with feature importance metrics confirming that “helplessness” was the most critical individual predictor, independently accounting for of the model’s out-of-sample predictive accuracy. Targeted clinical interventions that specifically dismantle the catastrophic cognition of helplessness may prove more efficacious in reducing somatic symptom severity than broad treatments aimed at generalized negative affect.
Downloads
References
Amiri, Z., & Amiri, Z. (2016). Assessment of a prediction model of depression based on disease perception and sleep quality mediated by pain catastrophizing in diabetic patients [Research]. Journal of Diabetes Nursing, 4(2), 48-58. http://jdn.zbmu.ac.ir/article-1-181-en.html
Asanova, A., Хаустова, О., Skrynnyk, O., & Mukharovska, I. (2025). Psychological, Clinical and Socio-Demographic Predictors of Pain Catastrophizing in Chronic Pain Patients: Insights From a Cross-Sectional Study. International Neurological Journal, 20(8), 411-421. https://doi.org/10.22141/2224-0713.20.8.2024.1124
Darnall, B. D., & Sazie, E. (2012). Pain Characteristics and Pain Catastrophizing in Incarcerated Women With Chronic Pain. Journal of Health Care for the Poor and Underserved, 23(2), 543-556. https://doi.org/10.1353/hpu.2012.0042
Doménech, J., Angulo, A. E., Peñalver-Barrios, L., Rio-González, E. D., Herrero, R., García‐Palacios, A., Díaz, M. M., Garreta-Catalá, I., Díez-Ulloa, M.-A., & Baños-Rivera, R. M. (2025). Catastrophizing and Fear Avoidance Beliefs in Chronic Low Back Pain: A Cross-Sectional Study. European Journal of Physical and Rehabilitation Medicine, 61(2). https://doi.org/10.23736/s1973-9087.25.08419-9
Edwards, R. R., Cahalan, C., Mensing, G., Smith, M., & Haythornthwaite, J. A. (2011). Pain, catastrophizing, and depression in the rheumatic diseases. Nature Reviews Rheumatology, 7(4), 216-224. https://doi.org/10.1038/nrrheum.2011.2
Goodin, B. R., McGuire, L., Stapleton, L. M., Quinn, N. B., Fabian, L. A., Haythornthwaite, J. A., & Edwards, R. R. (2009). Pain Catastrophizing Mediates the Relationship Between Self-Reported Strenuous Exercise Involvement and Pain Ratings: Moderating Role of Anxiety Sensitivity. Psychosomatic Medicine, 71(9), 1018-1025. https://doi.org/10.1097/psy.0b013e3181bc62ba
Heule, M. (2025). Adverse Childhood Experiences and Urogenital Pain: Examining the Mediating Effects of Negative Affect and Pain Catastrophizing. Neurourology and Urodynamics. https://doi.org/10.1002/nau.70022
Leung, L. C. (2012). Pain Catastrophizing: An Updated Review. Indian Journal of Psychological Medicine. https://doi.org/10.4103/0253-7176.106012
Ling, W. (2024). Pain Sensitivity and Acute Postoperative Pain in Patients Undergoing Abdominal Surgery: The Mediating Roles of Pain Self-Efficacy and Pain Catastrophizing. Pain Management Nursing, 25(2), e108-e114. https://doi.org/10.1016/j.pmn.2023.12.001
McWilliams, L. A., & Holmberg, D. (2010). Adult Attachment and Pain Catastrophizing for Self and Significant Other. Pain, 149(2), 278-283. https://doi.org/10.1016/j.pain.2010.02.019
Mir Ahmadi, Z., Khezri Moghadam, N., & Rahmati, A. (2022). Predicting pain catastrophizing based on psychological resilience and mindfulness in patients with cancer: mediating role of positive emotions [Research]. Shenakht Journal of Psychology and Psychiatry, 9(5), 130-141. https://doi.org/10.32598/shenakht.9.5.130
Moreira, M. F., & Oliveira, M. A. P. (2025). Exploring the interplay between catastrophizing and endometriosis pain through 2-wave and intensive longitudinal data. Pain Medicine, 26(4), 207-215. https://doi.org/10.1093/pm/pnae132
Ogawa, M., Saito, A., Karukivi, M., & Lahti, S. (2024). Associations of Sensory Sensitivity, Pain Catastrophizing, and Alexithymia With Dental Anxiety. European Journal of Oral Sciences, 132(2). https://doi.org/10.1111/eos.12973
Ong, A. D., Zautra, A. J., & Reid, M. C. (2010). Psychological resilience predicts decreases in pain catastrophizing through positive emotions. Psychology and Aging, 25(3), 516-523. https://doi.org/10.1037/a0019384
Stein, A., Johnson, B. N., Kelly, A. G., Cheavens, J. S., & McKernan, L. C. (2025). Negative Affect and Pain Catastrophizing Link Borderline Personality Disorder to Pain: Replicating and Extending the Borderline Personality Disorder–pain Association. Personality Disorders Theory Research and Treatment, 16(2), 173-183. https://doi.org/10.1037/per0000704
Sullivan, M. J. L., Lynch, M. E., & Clark, A. J. (2005). Dimensions of catastrophic thinking associated with pain experience and disability in patients with neuropathic pain conditions. Pain, 113(3). https://journals.lww.com/pain/fulltext/2005/02000/dimensions_of_catastrophic_thinking_associated.10.aspx
Trudel, P., & Cormier, S. (2024). Intolerance of uncertainty, pain catastrophizing, and symptoms of depression: a comparison between adults with and without chronic pain. Psychology, Health & Medicine, 29(5), 951-963. https://doi.org/10.1080/13548506.2023.2240073
Wren, A. A., Somers, Tamara J, Wright, Melissa A, Goetz, Mark C, Leary, Mark R, Fras, Anne Marie, Huh, Billy K, Rogers, Lesco L, Keefe, Francis J. (2012). Self-Compassion in Patients With Persistent Musculoskeletal Pain: Relationship of Self-Compassion to Adjustment to Persistent Pain. Journal of Pain and Symptom Management, 43(4), 759-770. https://doi.org/10.1016/j.jpainsymman.2011.04.014
Yamin, J. B. (2025). Childhood Abuse and Health Outcomes in Patients With Fibromyalgia: A Cross-Sectional Exploratory Study of the Moderating Effects of Pain Catastrophizing and Mindfulness. BMC Musculoskeletal Disorders, 26(1). https://doi.org/10.1186/s12891-025-08449-7
Ying Zhou, B. S. N. (2024). Relationship between pain resilience and pain catastrophizing in older patients after total knee arthroplasty: Chain-mediating effects of cognitive emotion regulation and pain management self-efficacy. Geriatric Nursing, 59, 571-580. https://doi.org/10.1016/j.gerinurse.2024.08.011
Zare, H., Mohammadi, N., Motaghi, P., Afshar, H., & Pourkazem, T. (2014). Treatment effect of modified cognitive therapy based on mindfulness, catastrophizing, acceptance and pain intensity of affected patients with fibromyalgia. Health Psychology, 3(4), 113-194.