Modeling the Contribution of Cognitive Fusion, Rumination, and Worry to Psychosomatic Distress: An Explainable Machine Learning Study
Keywords:
Psychosomatic distress, Cognitive fusion, Rumination, Worry, Explainable machine learningAbstract
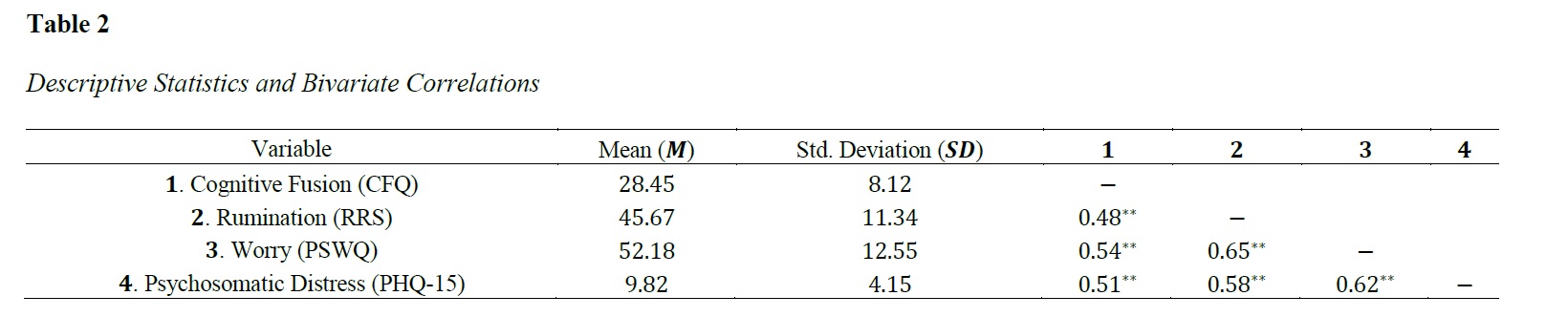
The present study aimed to model the unique and interactive contributions of cognitive fusion, rumination, and worry to psychosomatic distress within a Tunisian adult sample by applying and interpreting an explainable machine learning framework. A cross-sectional design was utilized to evaluate 1254 adult participants (M_age=32.4, SD=8.7) from Tunisia, recruited via snowball sampling. Self-report data were collected using the Cognitive Fusion Questionnaire (CFQ), Ruminative Responses Scale (RRS), Penn State Worry Questionnaire (PSWQ), and Patient Health Questionnaire-15 (PHQ-15). The data analysis employed an advanced machine learning pipeline, comparing Random Forest, Support Vector Regression, and eXtreme Gradient Boosting (XGBoost) algorithms. The optimal model was subsequently interpreted using the SHapley Additive exPlanations (SHAP) framework to extract global feature importance, non-linear thresholds, and interaction effects. Bivariate correlations demonstrated significant positive associations between all cognitive variables and psychosomatic distress (r=0.51 to 0.62). The XGBoost algorithm achieved the highest predictive performance (R^2=0.463, RMSE=2.41). SHAP global feature importance analysis ranked Worry as the top predictor of psychosomatic distress (Mean ∣SHAP∣=1.45), followed sequentially by Rumination and Cognitive Fusion. Furthermore, SHAP dependence plots revealed critical non-linear dynamics, identifying a specific threshold where worry scores exceeding 55 exponentially accelerated physical distress, as well as a significant interaction effect indicating that high cognitive fusion severely amplifies the detrimental somatic impact of rumination. Treating severe psychosomatic distress requires targeted interventions that rapidly reduce worry below critical severity thresholds and utilize cognitive defusion strategies to break the compounding cycle of rumination and psychological entanglement.
Downloads
References
Aghaziarati, A., Jun, H., & Dai, G.-S. (2024). Mind-Body Interactions in Chronic Pain Sufferers: A Qualitative Study on Personality Factors. Journal of Personality and Psychosomatic Research (JPPR), 1(3), 27-33. https://doi.org/10.61838/kman.jppr.1.3.5
Alsaffar, K. F. (2023). Overexcitability and Its Impact on Psychosomatic Disorders and the Role of "Cognitive Emotion Regulation" as a Mediating Variable. https://doi.org/10.21203/rs.3.rs-2397392/v1
Bermpohl, F. M. g., & Martin, A. (2025). Efficacy of Cognitive Behavioral Therapy and Acceptance- And Mindfulness-Based Treatments in Adults With Bodily Distress: A Network Meta-Analysis. Psychotherapy and psychosomatics, 94(3), 207-224. https://doi.org/10.1159/000544825
Denovan, A., Dagnall, N., & Lofthouse, G. (2018). Neuroticism and Somatic Complaints: Concomitant Effects of Rumination and Worry. Behavioural and Cognitive Psychotherapy, 47(4), 431-445. https://doi.org/10.1017/s1352465818000619
Emamzadeh, Z., Rahimian Bugar, E., & Mashhadi, A. (2023). The effectiveness of contextual schema therapy on emotion regulation and painful somatic symptoms in individuals with social anxiety disorder: A single-case study. Journal of Cognitive Psychology and Psychiatry, 10(3), 1-16. https://doi.org/10.32598/shenakht.10.3.1
Farahi, S., Naziri, G., Davodi, A., & Fath, N. (2023). The Mediating Role of Cognitive Emotion Regulation Strategies in the Relationship Between Early Maladaptive Schemas, Alexithymia, and Emotional Intelligence With Somatic Symptoms in People With Somatic Symptoms Disorder. Practice in Clinical Psychology, 11(3), 187-200. https://doi.org/10.32598/jpcp.11.3.887.1
Farhadi Navroud, S., Tahmoursi, N., & Sedaghat, M. (2023). A comparison of the effectiveness of mindfulness-based therapy and cognitive-behavioral therapy on negative automatic thoughts in university entrance exam volunteers with somatic symptoms. Rooyesh-e-Ravanshenasi (Psychological Growth), 12(1), 155-166. http://frooyesh.ir/article-1-3690-fa.html
Gasparre, D., Pepe, I., Laera, D., Abbatantuono, C., De, M. F., Taurino, A., D’Erasmo, D., Fanizzi, P., Antonucci, L. A., Pantaleo, A., Cavallaro, G., Pontillo, V., Taurisano, P., & Quaranta, N. (2023). Cognitive Functioning and Psychosomatic Syndromes in a Subjective Tinnitus Sample. Frontiers in psychology, 14. https://doi.org/10.3389/fpsyg.2023.1256291
Hertenstein, E., Trinca, E., Schneider, C. L., Fehér, K. D., Johann, A. F., & Nissen, C. (2024). Acceptance and Commitment Therapy, Combined with Bedtime Restriction, versus Cognitive Behavioral Therapy for Insomnia: A Randomized Controlled Pilot Trial. Psychotherapy and psychosomatics, 93(2), 114-128. https://doi.org/10.1159/000535834
Kiani Rad, M. (2024). Effectiveness of Cognitive Behavioral Therapy on Body Image Concern in Women with Depression Symptoms. Journal of Psychological Dynamics in Mood Disorders (PDMD), 3(1), 124-138. https://doi.org/10.22034/pdmd.2024.434757.1039
Kopf-Beck, J., Müller, C. L., Tamm, J., Fietz, J., Rek, N., Just, L., & Egli, S. (2024). Effectiveness of Schema Therapy versus Cognitive Behavioral Therapy versus Supportive Therapy for Depression in Inpatient and Day Clinic Settings: A Randomized Clinical Trial. Psychotherapy and psychosomatics, 1-12. https://doi.org/10.1159/000535492
Law, M., Pickering, I., Bartlett, E., Sebaratnam, G., Varghese, C., Gharibans, A., O'Grady, G., Andrews, C. N., & Calder, S. (2023). Cognitive behavioural therapy-based interventions for gastroduodenal disorders of gut-brain interaction: A systematic review. Journal of psychosomatic research, 111516. https://doi.org/10.1016/j.jpsychores.2023.111516
Ludwikowska-Świeboda, K. (2023). Rumination About the Death of a Spouse Versus the Severity of Somatic Symptom Disorder and Sleep Disturbances in Widowed Individuals in Late Adulthood. Current Problems of Psychiatry, 24, 114-124. https://doi.org/10.12923/2353-8627/2023-0011
Lundberg, K. (2023). The effect of mindfulness-based cognitive therapy on alexithymia in fibromyalgia: A randomized controlled trial. Journal of psychosomatic research, 165, 111156.
Mehrmanesh, E., Hafezi, F., Ehteshamzadeh, P., & Bakhtiarpour, S. (2023). Comparing the effectiveness of cognitive behavioral therapy, biofeedback and EMDR on anxiety sensitivity in women with migraine. Journal of Personality and Psychosomatic Research (JPPR), 1(1), 10-14. https://doi.org/10.61838/kman.jppr.1.1.3
Rostami, M., Bulut, S., Coelho, O., & Riyono, B. (2024). Living with Fibromyalgia: A Phenomenological Study of Pain, Fatigue, and Coping. Journal of Personality and Psychosomatic Research (JPPR), 2(1), 16-23. https://doi.org/10.61838/kman.jppr.2.1.4
Seyed Alitabar, S. H., & Goli, F. (2024). Exploring the Predictive Role of Body Image and Rumination on Somatic Symptom Severity: A Quantitative Analysis. International Journal of Body, Mind and Culture, 11(3), 193-200. https://doi.org/10.22122/ijbmc.v11i3.689
Shahverdi, A., Omidi, M., & Nik, M. M. (2023). Effect of Mindfulness-Based Cognitive Therapy on Cognitive Emotion Regulation, Psychosomatic Symptom Severity of Migraine, and Stress Coping Styles of Women With Migraine. Iranian Journal of Psychiatry and Clinical Psychology, 29(1), 18-31. https://doi.org/10.32598/ijpcp.29.1.4414.1
Sharpe, L., Bisby, M. A., Menzies, R. E., Boyse, J. B., Richmond, B., Todd, J., Sesel, A. L., & Dear, B. F. (2025). A Tale of Two Treatments: A Randomized Controlled Trial of Mindfulness or Cognitive Behaviour Therapy Delivered Online for People with Rheumatoid Arthritis. Psychotherapy and psychosomatics, 94(2), 89-100. https://doi.org/10.1159/000542489
Shkëmbi, F. (2023). "Mindfulness, Somatic and Cognitive Symptoms of Anxiety, and Self-Esteem: A Randomized Controlled Trial". https://doi.org/10.36315/2023inpact076
Smith, O. R., Aarø, L. E., & Knapstad, M. (2023). The importance of symptom reduction for functional improvement after cognitive behavioral therapy for anxiety and depression: A causal mediation analysis. Psychotherapy and psychosomatics, 92(3), 193-202. https://doi.org/10.1159/000530650
Walsh, E. A., Boland, Cody L, Popok, Paula J, Pedreira, Patricia B, Fox, Rina S, Moreno, Patricia I, Yanez, Betina, Penedo, Frank J. (2023). Marital status and perceived stress in men with advanced prostate cancer: A randomized-controlled trial of cognitive behavioral stress management. Journal of psychosomatic research, 167, 111198. https://doi.org/10.1016/j.jpsychores.2023.111198
Wong, S. Y. S., Chan, S. K. C., Yip, B. H. K., Wang, W., Lo, H. H. M., Zhang, D., & Bögels, S. M. (2023). The effects of mindfulness for youth (MYmind) versus group cognitive behavioral therapy in improving attention and reducing behavioral problems among children with attention-deficit hyperactivity disorder and their parents: A randomized controlled trial. Psychotherapy and psychosomatics, 92(6), 379-390. https://doi.org/10.1159/000534962
Wong, S. Y. S., Chan, S. K. C., Yip, B. H. K., Wang, W., Lo, H. H. M., Zhang, D., & Bögels, S. M. (2024). The effects of mindfulness for youth (MYmind) versus group cognitive behavioral therapy in improving attention and reducing behavioral problems among children with ADHD and their parents: a randomized controlled trial. Psychotherapy and psychosomatics, 92(6), 379. https://doi.org/10.1159/000534962
Xu, L., & Shi, Y. (2024). Addressing psychosomatic symptom distress with mindfulness-based cognitive therapy in somatic symptom disorder: Mediating effects of self-compassion and alexithymia. Frontiers in Psychiatry, 15. https://doi.org/10.3389/fpsyt.2024.1289872
Yildiz Karaahmet, A., Bilgiç, F. S., Yilmaz, T., & Shafaati Laleh, S. (2025). The effects of cognitive interventions on quality of life in infertile women: A meta-analysis of randomized controlled trials. Journal of Psychosomatic Obstetrics and Gynaecology, 46(1), 2560828. https://doi.org/10.1080/0167482X.2025.2560828
Zulkifli, N., Abalorio, B., & Muñoz, N. G. (2025). Cognitive Avoidance and Somatic Complaints in Adolescents: The Mediating Role of Interoceptive Awareness. Jayps, 6(1), 156-165. https://doi.org/10.61838/kman.jayps.6.1.17