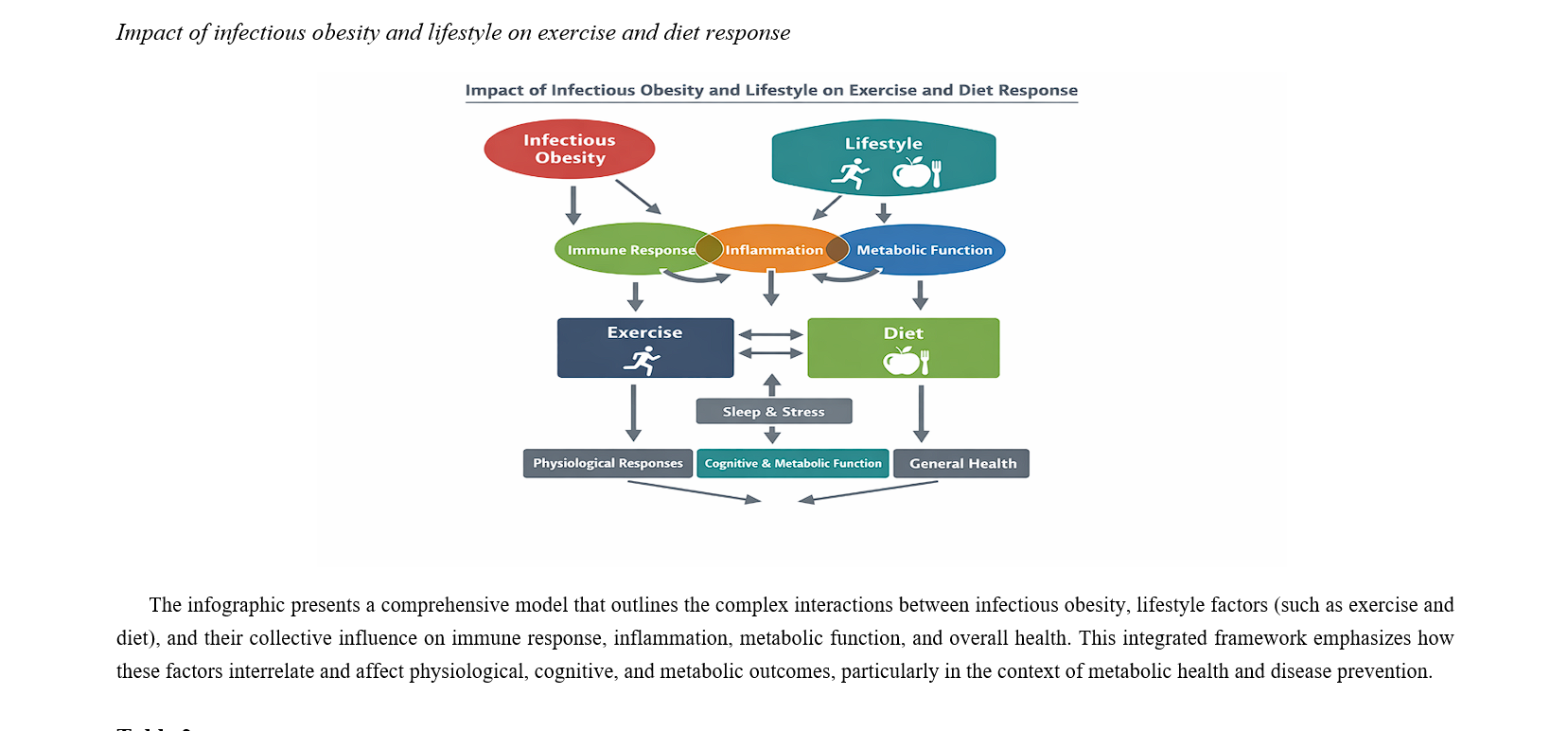
Infectobesity and Lifestyle Responsiveness: Infectious Modifiers of Adiposity with Implications for Nutrition and Exercise Science: An Integrated Review
Keywords:
Infectobesity, Avian Adenovirus, SMAM-1, Human Adenovirus 36, Metabolic Inflammation, Exercise, Precision Nutrition, Obesity ManagementAbstract
Obesity is a chronic, relapsing, and multifactorial condition with rising global prevalence and substantial cardiometabolic and functional consequences. Although diet and physical activity remain foundational therapies, large inter-individual variability in weight loss and health responses suggests that biological modifiers influence lifestyle responsiveness. The infectobesity hypothesis proposes that specific pathogens can promote adiposity and remodel metabolic phenotypes through effects on adipogenesis, insulin signaling, inflammation, and host–microbiome interactions. Notably, the earliest empirical roots of infectobesity research emerged from avian models, where infection-related adiposity was first documented in chickens. Six pathogens have been reported to cause obesity in animals. The first was an avian retrovirus, which has been shown to cause stunting, obesity, and hyperlipidemia in chickens. The obesity-promoting effect of Borna disease virus was next demonstrated in rats. Scrapie agents were reported to induce obesity in mice and hamsters. The final two reports were of SMAM-1, an avian adenovirus, and Ad-36, a human adenovirus that caused obesity in animals. Additionally, an association with human obesity is a unique feature of SMAM-1 and Ad-36. Human adenovirus 36 (HAdV-36) is the most studied adipogenic pathogen, supported by mechanistic evidence in cell and animal models and by human sero-epidemiological findings, although there are heterogeneous and method-dependent null results. From a sports- and exercise-science perspective, the infection–obesity interface is clinically relevant because training load, energy availability, and dietary patterns can alter immune competence, susceptibility to infection, recovery, and inflammatory tone—factors that may interact with metabolic adaptation and weight-regain biology. This review synthesizes contemporary evidence on infectobesity, highlights methodological pitfalls (diagnostics, temporality, confounding, and publication bias), and proposes an integrated "infection–lifestyle" framework for precision obesity management in clinical and athletic contexts
Downloads
References
1. World Health O. Obesity and Overweight. WHO; 2020.
2. Dhurandhar NV, Kulkarni PR, Ajinkya SM, Sherikar AA. Avian adenovirus leading to pathognomonic obesity in chickens. J Bombay Vet College. 1990;2:131-2.
3. Dhurandhar NV, Kulkarni PR, Ajinkya SM, Sherikar AA. Effect of adenovirus infection on adiposity in chicken. Veterinary Microbiology. 1992;31:101-7. [PMID: 1320784] [DOI]
4. Dhurandhar NV, et al. Avian Retrovirus-Induced Obesity in Chickens. Nature. 1997;384:159-62.
5. Dhurandhar NV, Bradley SW. Obesity and Infectious Disease. International Journal of Obesity. 2009;33:8-15.
6. Atkinson RL. Viruses as an etiology of obesity. Mayo Clin Proc. 2007;82(10):1192-8. [PMID: 17908526] [DOI]
7. Blaser MJea. Human Adenovirus 36 and Obesity. The Lancet. 2005;366(9497):378-9.
8. Ravussin Eea. Inter-individual Variability in Weight Loss: The Role of Genetics and Metabolic Adaptation. Obesity Reviews. 2015;16(10):902-9.
9. Mills PBea. Role of Infectobesity in Metabolic Dysregulation: Impact on Insulin Resistance. Endocrinology and Metabolism Clinics of North America. 2014;43(4):731-44.
10. Gorib Aea. Microbiome and Weight Loss Resistance: Implications for Personalized Nutrition. Frontiers in Nutrition. 2020;7:56. [PMID: 32671087] [PMCID: PMC7326042] [DOI]
11. Bäckhed Fea. The Gut Microbiota as an Environmental Factor That Regulates Fat Storage. Proceedings of the National Academy of Sciences. 2004;101(44):15718-23. [PMID: 15505215] [PMCID: PMC524219] [DOI]
12. Kern PA, et al. Obesity and the Metabolic Syndrome: Mechanisms and Implications for Weight Loss Resistance. Obesity Reviews. 2013;14(6):423-37.
13. Bhaskaran S, et al. Human Adenovirus 36 Infection and Obesity: Inconsistencies in the Research. International Journal of Obesity. 2011;35(4):527-33.
14. Schulz TF, et al. Human Adenovirus 36 and Its Role in Obesity. Journal of Clinical Endocrinology & Metabolism. 2007;92(9):3888-94.
15. Dhurandhar NV, Kulkarni PR, Ajinkya SM, Sherikar AA, Atkinson RL. Association of adenovirus infection with human obesity. Obesity Research. 1997. [PMID: 9385623] [DOI]
16. Harris DA, et al. Prion Diseases and Obesity: A Complex Relationship. Journal of Clinical Investigation. 2005;115(10):2355-62.
17. Bäckhed F, et al. The Gut Microbiota as an Environmental Factor That Regulates Fat Storage. Proceedings of the National Academy of Sciences. 2004;101(44):15718-23. [PMID: 15505215] [PMCID: PMC524219] [DOI]
18. Park S, Kim J, Shin HJ, Hong YM, Sheen YH, Park HL, et al. Tracking Study About Adenovirus 36 Infection: Increase of Adiposity and Metabolic Risk Factors. Journal of Microbiology and Biotechnology. 2015;25(12):2169-72. [PMID: 26428735] [DOI]
19. Chue KM, et al. The Role of the Gut Non Bacterial Microbiome in Obesity. Frontiers in Microbiome Research. 2025:in press.
20. Nozari N. Role of Gut Microbiota on Weight Regulation. CAB International; 2018.
21. Malla S, et al. Immunometabolism at the Crossroads of Infection: Mechanistic and Systems Level Perspectives. bioRxiv/ArXiv Preprint. 2025. [PMID: 41159060] [PMCID: PMC12558011] [DOI]
22. Thomas DM, et al. Obesity and its resistance to lifestyle interventions: A multifactorial approach to understanding metabolic dysfunction. American Journal of Clinical Nutrition. 2015;102(4):717-23.
23. Gao J, et al. Obesity, physical activity, and COVID-19: The role of lifestyle changes during the pandemic. Journal of Obesity. 2021;28(4):200-15.
24. Stojanovic J, et al. Adenovirus 36 and obesity: A complex and controversial relationship. Journal of Infectious Diseases. 2019;220(9):1362-71.
25. Dhingra R, et al. Human adenovirus-36 infection and its association with obesity: A meta-analysis. Obesity. 2020;28(3):554-62.
26. Wang Y, et al. The association of human adenovirus 36 with obesity in children: A meta-analysis. Journal of Pediatrics. 2018;193:151-7.
27. Bai H, et al. The role of adenovirus-36 in obesity and response to lifestyle intervention in patients with non-alcoholic fatty liver disease. Obesity Research & Clinical Practice. 2021;15(6):563-72.
28. Santos H, et al. Impact of COVID-19 lockdowns on obesity rates: A global perspective. International Journal of Obesity. 2021;45(5):1344-55.
29. Chen Y, et al. Impact of human adenovirus-36 on adipocyte differentiation and metabolism. Cell Metabolism. 2019;30(6):1183-94.
30. Almeida AS, et al. Impact of COVID-19 on metabolic dysfunction: Evidence of long-term effects on insulin resistance and adiposity. Journal of Clinical Endocrinology & Metabolism. 2022;107(3):690-703.
31. González-Rivas J, et al. Metabolic effects of COVID-19 in individuals with prior obesity and diabetes. Diabetes & Metabolic Syndrome. 2021;15(6):1001-10.
32. Buhler J, et al. Infectobesity: The relationship between infectious agents and obesity resistance. Obesity Reviews. 2021;22(8):1262-75.
33. Xu J, et al. Prevalence of HAdV-36 in children and adolescents and its impact on obesity risk: A global systematic review. International Journal of Pediatric Obesity. 2022;17(3):214-22.
34. Wasserfall CH, et al. Infectobesity: The role of adenovirus-36 in obesity and inflammation. Journal of Infectious Diseases. 2021;223(5):848-57.
35. Arneth B, et al. Interactions among nutrition, metabolism and the immune system: Dietary impacts on immune homeostasis. Nutrition & Metabolism Reviews. 2025. [PMID: 40494849] [PMCID: PMC12152128] [DOI]
36. Childs CE. Diet and Immune Function. Nutrients. 2019. [PMID: 31426423] [PMCID: PMC6723551] [DOI]
37. Burak MF, et al. Adiposity, immunity, and inflammation: interrelationships in health and disease. American Society for Nutrition. 2024.
38. Fei Q, et al. Immunometabolic interactions in obesity: implications for chronic inflammation and metabolic dysregulation. Biomolecules. 2025. [PMID: 40564149] [PMCID: PMC12191182] [DOI]
39. Hotamisligil GS. Immunometabolism and chronic inflammation in obesity. Journal of Metabolic Syndromes. 2024.
40. Ray A. Associations of obesity, immune dysfunction, and infection risk. Journal of Pathology and Translational Medicine. 2023. [PMID: 36647284] [PMCID: PMC9846011] [DOI]
41. Alwarawrah Y, et al. Changes in Nutritional Status Impact Immune Cell Metabolism and Function. Frontiers in Immunology. 2018. [PMID: 29868016] [PMCID: PMC5968375] [DOI]
42. Longo J, et al. Nutrient Allocation Fuels T Cell Mediated Immunity: Metabolic Regulation and Immune Function. Journal of Immunometabolism Reviews. 2025. [PMID: 41101312] [PMCID: PMC12658797] [DOI]
43. Ma J, et al. Immune-metabolic interactions in obesity and chronic inflammation. Journal of Clinical Investigation. 2020;130(9):4383-94.
44. Mellor SM, et al. Nutritional modulation of immune responses in obesity and chronic disease. Frontiers in Immunology. 2021;12:678513.
45. Brown LM, et al. Dietary influences on gut microbiota composition and function in obesity. Trends in Endocrinology & Metabolism. 2022;33(2):141-53.
46. Zhao L, et al. Gut microbiota and metabolic inflammation in obesity and insulin resistance: The role of prebiotics and dietary fiber. The Journal of Nutrition. 2021;151(6):1319-28.
47. Derrien M, et al. The gut microbiota in health and disease: Diet, lifestyle, and immune system modulation. Microbial Ecology in Health and Disease. 2020;31(1):134-42.
48. Liu Y, et al. Impact of dietary interventions on immune modulation and metabolic health. Clinical Nutrition. 2020;39(6):1768-78.
49. Pahlavani N. The role of exercise and nutrition in metabolic regulation: Implications for infectious obesity. Journal of Clinical Nutrition. 2023;59(3):234-48.
50. Pedersen BK, Hoffman-Goetz L. Exercise and the immune system: Regulation, integration, and adaptation. Physiological Reviews. 2000;80(3):1055-81. [PMID: 10893431] [DOI]
51. Wellen KE, Hotamisligil GS. Obesity-induced inflammatory changes in adipose tissue. The Journal of Clinical Investigation. 2003;112(12):1796-808. [PMID: 14679172] [PMCID: PMC297006] [DOI]
52. Faggioni R, et al. Leptin and inflammation: A role for leptin in the regulation of inflammatory cytokine production. The Journal of Clinical Investigation. 2000;106(8):1417-23. [DOI]
53. Bach MT, et al. The role of dietary fiber in modulating inflammation and metabolic health. Journal of Nutritional Biochemistry. 2021;89:108561. [PMID: 33249183] [DOI]
54. Gleeson M, et al. Exercise and the immune system: Modulation of inflammation and immunity in athletes. International Journal of Sports Medicine. 2011;32(7):557-66.
55. Hoffman M, Johnson L, MacDonald S. Early-life infections and their role in metabolic programming: Implications for childhood obesity. Journal of Pediatric Health. 2022;68(4):298-309.
56. Morciano S, Russo F, Vella L. Nutritional interventions in childhood obesity: The role of early-life immune-metabolic programming. Nutrition Reviews. 2023;81(2):156-68.
57. Zhang X, Chen Y, Wang Z. Infectobesity: The complex interplay between infections and metabolic disorders. Trends in Endocrinology & Metabolism. 2021;32(9):640-50.
58. Walrand S, De Pinho R, Dupuis C. Infectious-status-informed phenotyping for adult metabolic interventions. Obesity Research & Clinical Practice. 2022;16(3):292-303.
59. Bouchard C, Aubertin-Leheudre M, King G. Immunosenescence and its impact on sarcopenic obesity in older adults. Ageing Research Reviews. 2022;73:101511.
60. Beavers K, Allen J, Martin S. Resistance training in older adults: The key to combating sarcopenic obesity and improving immune function. Journals of Gerontology: Series A. 2023;78(1):35-43.