Machine Learning–Based Discovery of Hidden Behavioral Profiles Underlying High-Performing Innovation Teams
Keywords:
Innovation teams, behavioral profiles, machine learning, organizational behavior, innovation performance, XGBoost, psychological safety, team dynamicsAbstract
Objective: The objective of this study was to identify latent behavioral profiles underlying innovation teams and examine their predictive relationship with innovation performance using advanced machine learning techniques.
Methods and Materials: This quantitative cross-sectional study was conducted among 574 employees from 84 formally designated innovation teams across technology, engineering, biotechnology, finance, and advanced manufacturing organizations in Singapore. Data were collected using validated multi-item instruments measuring collaborative orientation, psychological safety, knowledge sharing, intrinsic motivation, proactive problem solving, learning orientation, adaptive flexibility, creative self-efficacy, and collective efficacy. Team innovation performance was assessed through both leader-rated evaluations and objective performance indicators. A multi-phase machine learning pipeline was implemented, including data normalization, dimensionality reduction, unsupervised clustering using Gaussian mixture models, and supervised prediction using Random Forest and XGBoost algorithms. Model robustness was evaluated through five-fold cross-validation, out-of-sample testing, and feature importance analysis using SHAP values.
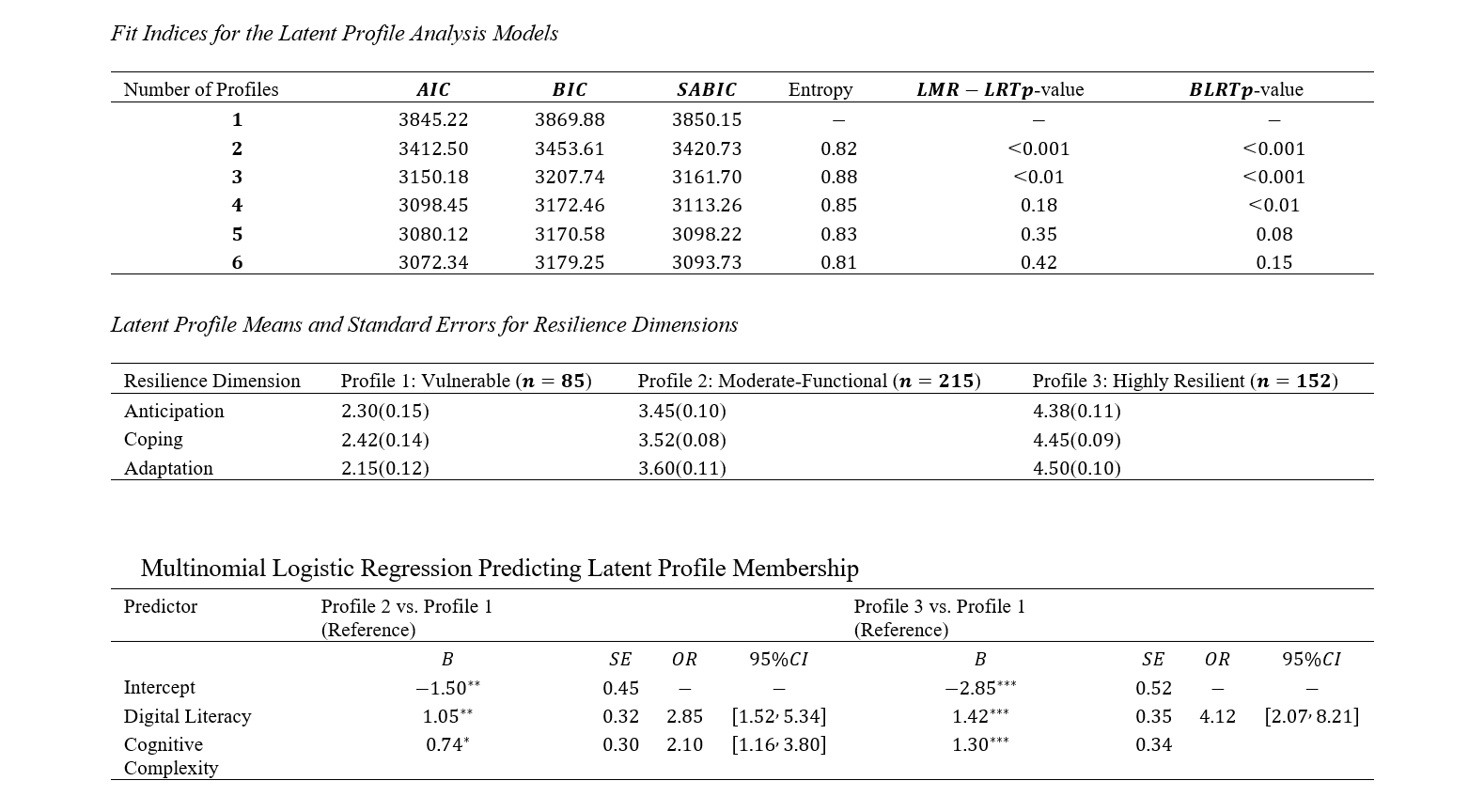
Findings: Unsupervised learning revealed four statistically distinct behavioral profiles that significantly differed in innovation performance. XGBoost achieved the highest predictive accuracy (93%), with strong discriminative power (AUC = 0.96). The Synergistic Innovators profile demonstrated significantly higher innovation outcomes than all other profiles (p < .001). Feature importance analysis identified intrinsic motivation, collaborative orientation, psychological safety, proactive problem solving, and knowledge sharing as the strongest predictors of innovation performance.
Conclusion: The findings demonstrate that innovation performance emerges from coherent behavioral configurations rather than isolated behavioral factors, and that machine learning provides a powerful framework for uncovering and predicting these hidden structures within organizational teams.
Downloads
References
Akl, A., Mohiyaldeen, I., Alshatti, R., Alenezi, O., Dougherty, R. J., Al-Raihan, A., Alotaibi, S., Tadros, N., & Longenecker, J. C. (2022). The Prevalence of Burnout and Its Associated Factors Among Surgical Specialists in Kuwait Ministry of Health Hospitals. Frontiers in Public Health, 10. https://doi.org/10.3389/fpubh.2022.679834
Barnes, C. M., Wagner, D. T., Schabram, K., & Boncoeur, D. (2022). Human Sustainability and Work: A Meta-Synthesis and New Theoretical Framework. Journal of Management, 49(6), 1965-1996. https://doi.org/10.1177/01492063221131541
Cildoz, M., Ibarra, A., & Mallor, F. (2023). Acuity-Based Rotational Patient-to-Physician Assignment in an Emergency Department Using Electronic Health Records in Triage. Health Informatics Journal, 29(2). https://doi.org/10.1177/14604582231167430
Coffee, Z. (2025). Trauma-Related Stress and Resilience in a Multistate Sample of Methadone Treatment Staff. Substance Use Research and Treatment, 19. https://doi.org/10.1177/29768357251383239
Devery, K., Winsall, M., & Rawlings, D. (2022). Teams and Continuity of End-of-Life Care in Hospitals: Managing Differences of Opinion. BMJ Open Quality, 11(2), e001724. https://doi.org/10.1136/bmjoq-2021-001724
Dong, F., Huang, W., Chu, C., Lv, L., & Zhang, M. (2023). Influence of Workplace Stress and Social Support on Humanistic Caring Ability in Chinese Nurses. Nursing Open, 10(6), 3603-3612. https://doi.org/10.1002/nop2.1606
Ehmidat, M., Dawabsha, K., Manasrah, A., Salameh, H., Khalili, H., Waleed, S., shanann, S., Abudaia, S., Jaber, M., sarahneh, h., Fakhouri, S., & Mohamed, S. A. (2025). Effect of Burnout Due to Heavy Workload on Surgical Residents: A Multi-National Cross-Sectional Study. https://doi.org/10.21203/rs.3.rs-7101378/v1
García, P., Stephen, P., Shah, S., Smith, M., Jeong, Y., Devon-Sand, A., Tai-Seale, M., Takazawa, K., Clutter, D., Vogt, K., Lugtu, C., Rojo, M., Lin, S., Shanafelt, T. D., Pfeffer, M. A., & Sharp, C. (2024). Artificial Intelligence–Generated Draft Replies to Patient Inbox Messages. JAMA Network Open, 7(3), e243201. https://doi.org/10.1001/jamanetworkopen.2024.3201
Irwan, I. (2024). Workplace Conflict: Its Impact on Employee Motivation and Productivity. Paradoks Jurnal Ilmu Ekonomi, 7(4), 481-494. https://doi.org/10.57178/paradoks.v7i4.993
Kuhns, J. B., Messer, S., & Exum, M. L. (2024). Process Mapping Homicide Investigations and Estimating Resource Requirements for Homicide Units: Findings From a Case Study in the United States. The Police Journal Theory Practice and Principles, 98(1), 197-220. https://doi.org/10.1177/0032258x241258363
Metersky, M. L., Rodrick, D., Ho, S. Y., Galusha, D., Timashenka, A., Grace, E. N., Marshall, D., Eckenrode, S., & Krumholz, H. M. (2024). Hospital COVID-19 Burden and Adverse Event Rates. JAMA Network Open, 7(11), e2442936. https://doi.org/10.1001/jamanetworkopen.2024.42936
Narciso, I., Albuquerque, S., & Nunes, S. (2024). Addiction Interprofessional Experiences of Care: Stress, Coping and Transformation. International journal of mental health nursing, 33(4), 928-936. https://doi.org/10.1111/inm.13289
Ooijen, W. B., Malfait, S., Waal, G. H., & Hafsteinsdøttir, T. B. (2023). Nurses' Motivations to Leave the Nursing Profession: A Qualitative Meta‐aggregation. Journal of Advanced Nursing, 79(12), 4455-4471. https://doi.org/10.1111/jan.15696
Prasad, K., McLoughlin, C., Stillman, M., Poplau, S., Goelz, E., Taylor, S., Nankivil, N., Brown, R., Linzer, M., Cappelucci, K., Barbouche, M., & Sinsky, C. A. (2021). Prevalence and Correlates of Stress and Burnout Among U.S. Healthcare Workers During the COVID-19 Pandemic: A National Cross-Sectional Survey Study. EClinicalMedicine, 35, 100879. https://doi.org/10.1016/j.eclinm.2021.100879
Reguera‐Carrasco, C., Fernández‐García, E., Alvarez, A. N., Jimenez‐García, V. M., Prada‐Rizoto, M., Corral‐Cortés, Á., & Barrientos‐Trigo, S. (2025). Nurse‐Related Complexity of Care Perceived by Critical Care Nurses: A Multicentre Qualitative Study. Nursing in Critical Care, 30(4). https://doi.org/10.1111/nicc.70100
Saputra, M., & Satrya, A. (2024). Burnout and Quality of Work Life on Job Performance: Mediating Role of Job Satisfaction Among Financial Services Employees. Financial Engineering, 2, 313-325. https://doi.org/10.37394/232032.2024.2.29
Shawahna, R., Maqboul, I., Ahmad, O., Al-Issawy, A., & Abed, B. (2022). Prevalence of Burnout Syndrome Among Unmatched Trainees and Residents in Surgical and Nonsurgical Specialties: A Cross-Sectional Study From Different Training Centers in Palestine. BMC Medical Education, 22(1). https://doi.org/10.1186/s12909-022-03386-8
Shih, K. K., Anderson, A. E., Dai, J., Fellman, B., Moraes, A. R. d., Stanton, P., Nelson, C. A., Cruz, V. D., & Bruera, É. (2023). Hybrid Work From Home Clinical Academic Environment: A One-Year Follow-Up Survey of Attitudes and Beliefs of Members of a Department of Palliative Care, Rehabilitation, and Integrative Medicine. Journal of Palliative Medicine, 26(3), 342-352. https://doi.org/10.1089/jpm.2022.0203
Taylor, G. A., Ayyala, R. S., & Coley, B. D. (2022). How Did We Get Here? Thoughts on Health Care System Drivers of Pediatric Radiology Burnout. Pediatric Radiology, 52(6), 1019-1023. https://doi.org/10.1007/s00247-022-05318-6
Toqan, D., Ayed, A., & Khalaf, I. (2023). Effect of Progressive Muscle Relaxation Exercise on Anxiety Among Nursing Students Prior to Critical Care Clinical Training. Journal of Public Health Research, 12(2). https://doi.org/10.1177/22799036231181668
Wang, D., Hall, M. E. L., Shannonhouse, L., Mize, M. C., Aten, J. D., Davis, E. B., Tongeren, D. R. V., & Annan, K. (2021). Why Humility Is Vital to Effective Humanitarian Aid Leadership: A Review of the Literature. Disasters, 45(4), 797-818. https://doi.org/10.1111/disa.12446
Wolfe, A. H. J., Hinds, P. S., Arnold, R. M., Soghier, L., & Tompkins, R. (2022). Vulnerability of Inexperience: A Qualitative Exploration of Physician Grief and Coping After Impactful Pediatric Patient Deaths. Journal of Palliative Medicine, 25(10), 1476-1483. https://doi.org/10.1089/jpm.2022.0050
Zhao, B., Zhang, Z., & Zhang, M. (2025). Unlocking the Paradox: Exploring the Impact of Management Paradox Thinking on Corporate Innovation Performance. Sage Open, 15(3). https://doi.org/10.1177/21582440251359078