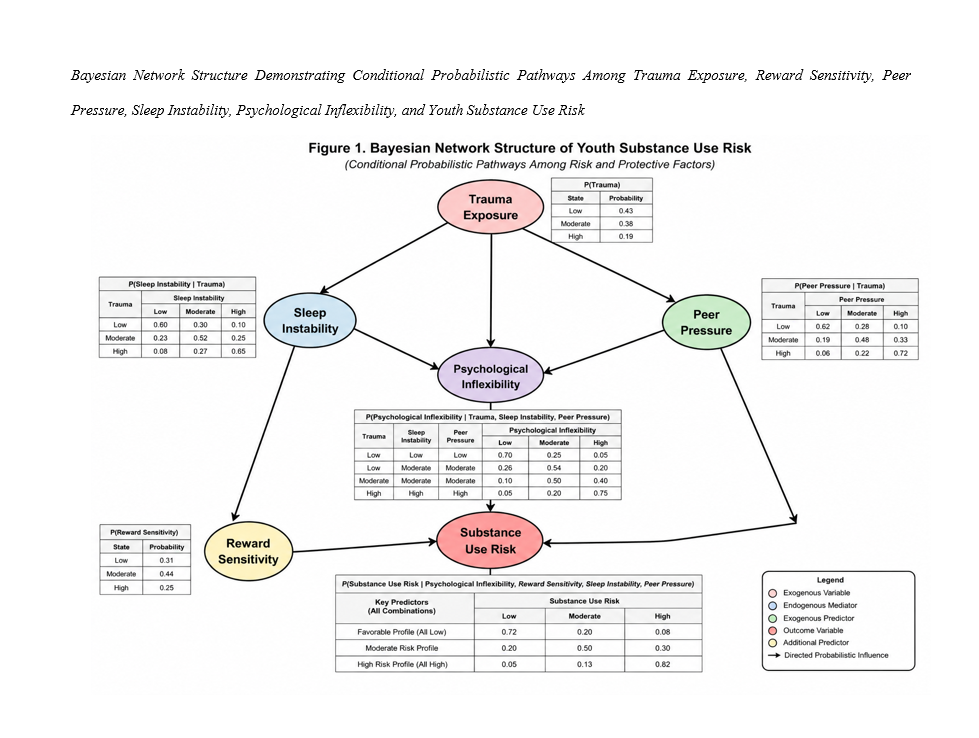
Bayesian Network Modeling of Youth Substance Use Risk Based on Trauma Exposure, Reward Sensitivity, Peer Pressure, Sleep Instability, and Psychological Inflexibility
Keywords:
Youth Substance Use, Bayesian Network Modeling, Trauma Exposure, Reward Sensitivity, Peer Pressure, Sleep Instability, Psychological Inflexibility, Adolescents, Emerging Adults, Predictive ModelingAbstract
Objective: The present study aimed to develop and evaluate a Bayesian network model for predicting youth substance use risk based on trauma exposure, reward sensitivity, peer pressure, sleep instability, and psychological inflexibility among adolescents and emerging adults in the United States.
Methods and Materials: This study employed a cross-sectional predictive modeling design using Bayesian probabilistic network analysis. The statistical population consisted of adolescents and emerging adults aged 15 to 22 years from educational institutions in the United States, from whom 1,248 participants were selected through multistage stratified sampling. Data were collected using the Substance Use Risk Profile Scale, Childhood Trauma Questionnaire-Short Form, Behavioral Activation System Scale, Peer Pressure Inventory, Sleep Condition Indicator, and Acceptance and Action Questionnaire-II. Data analysis was conducted using SPSS version 29 and Python 3.11. Bayesian network structure learning was implemented using the Hill-Climbing optimization algorithm with Bayesian Information Criterion scoring. Predictive performance was evaluated using classification accuracy, precision, recall, F1-score, sensitivity, specificity, and area under the receiver operating characteristic curve.
Findings: The findings demonstrated significant positive relationships among trauma exposure, reward sensitivity, peer pressure, sleep instability, psychological inflexibility, and substance use risk. Psychological inflexibility showed the strongest correlation with substance use risk (r = .65, p < .01), followed by trauma exposure (r = .61, p < .01). The Bayesian network model demonstrated high predictive performance with a training accuracy of 89.41%, testing accuracy of 86.93%, and area under the curve value of 0.91. Sensitivity analysis indicated that psychological inflexibility represented the strongest predictor within the network structure, followed by trauma exposure, peer pressure, reward sensitivity, and sleep instability. The probabilistic network further revealed that trauma exposure functioned as a central upstream variable influencing psychological inflexibility, peer pressure susceptibility, and sleep instability pathways associated with elevated substance use vulnerability.
Conclusion: The findings suggest that youth substance use vulnerability is shaped by a multidimensional network of emotional, cognitive, behavioral, and social risk mechanisms. Bayesian network modeling provided a powerful computational framework for identifying conditional dependency pathways among trauma exposure, reward sensitivity, peer pressure, sleep instability, psychological inflexibility, and substance use risk. The results highlight the importance of trauma-informed and multidimensional prevention strategies targeting emotional regulation, sleep health, peer influence processes, and psychological flexibility in adolescents and emerging adults.
Downloads
References
Adindu, K. N., Ajah, O. N., Ayowale, K. S., Onochie, E. D., Enemuo, N. R., & Okorie, C. D. (2024). Neuroscientific Approaches to Understanding Adolescent Susceptibility to Substance Abuse. International Neuropsychiatric Disease Journal, 21(6), 73-80. https://doi.org/10.9734/indj/2024/v21i6455
Akunna, G. G., & Lucyann, C. A. (2023). Nigeria’s War Against Drug Abuse: Prevalence, Patterns, Ramifications, Policy and Multisectoral Response, Strategies and Solutions. Studies in Social Science & Humanities, 2(10), 35-55. https://doi.org/10.56397/sssh.2023.10.06
Belfiore, C. I., Galofaro, V., Cotroneo, D., Lopis, A., Tringali, I., Denaro, V., & Casu, M. (2024). A Multi-Level Analysis of Biological, Social, and Psychological Determinants of Substance Use Disorder and Co-Occurring Mental Health Outcomes. Psychoactives, 3(2), 194-214. https://doi.org/10.3390/psychoactives3020013
Billieux, J., Bloch, J., Rochat, L., Fournier, L., Eben, C., Khazaal, Y., Simón, O., Andersen, M. M., King, D. L., & Lieberoth, A. (2023). 8th International Conference on Behavioral Addictions (ICBA 2023) August 23–25, 2023 Incheon, South Korea. Journal of Behavioral Addictions, 12(Supplement-1), 1-365. https://doi.org/10.1556/2006.2023.00800
Borodulin, N., & Holmberg, J. (2023). How Genetic and Sociocultural Factors Interact With Mental Health Disorders and Epigenetics to Predispose and Reinforce Substance Use Disorder. Journal of Student Research, 12(3). https://doi.org/10.47611/jsrhs.v12i3.5095
Bucklin, M. (2021). A 5-Factor Framework for Assessing Tobacco Use Disorder. Tobacco Use Insights, 14. https://doi.org/10.1177/1179173x21998355
Ćatović, A., & Gudelj, K. (2021). Characteristics of Psychoactive Substances Consumption Among Students of First and Fifth Year of Faculty of Medicine of Sarajevo University. GSC Advanced Research and Reviews, 06(03), 181-187. https://doi.org/10.30574/gscarr.2021.6.3.0058
Chang, R. S., Lee, M., Im, J. J., Choi, K. H., Kim, J., Chey, J., Shin, S.-H., & Ahn, W. Y. (2023). Biopsychosocial Factors of Gaming Disorder: A Systematic Review Employing Screening Tools With Well-Defined Psychometric Properties. Frontiers in Psychiatry, 14. https://doi.org/10.3389/fpsyt.2023.1200230
Chiappini, S., Sampogna, G., Ventriglio, A., Menculini, G., Ricci, V., Pettorruso, M., Volpe, U., & Martinotti, G. (2025). Exploring Emerging Psychopathological Characteristics and Challenges of Novel Depression Subtypes: Insights From the Literature. Frontiers in Psychiatry, 16. https://doi.org/10.3389/fpsyt.2025.1613251
Elisha, E., & Shachaf-Friedman, E. (2025). The Wounded Healer Paradox: Perceived Triggers of Drug Relapse and Recovery Among Peer Supporters. https://doi.org/10.21203/rs.3.rs-6517733/v1
Elvin, O. M., Modecki, K. L., & Waters, A. M. (2024). An Expanded Conceptual Framework for Understanding Irritability in Childhood: The Role of Cognitive Control Processes. Clinical Child and Family Psychology Review, 27(2), 381-406. https://doi.org/10.1007/s10567-024-00489-0
Flykt, M., Salo, S., & Pajulo, M. (2021). “A Window of Opportunity”: Parenting and Addiction in the Context of Pregnancy. Current Addiction Reports, 8(4), 578-594. https://doi.org/10.1007/s40429-021-00394-4
Groenewald, C. B., Palermo, T. M., Rabbitts, J. A., Flack, R. L., & Kreider, S. L. (2025). Teens and Opioids Postsurgery (TOPS): Protocol for a Prospective Observational Study Describing Associations Between Sleep Deficiency and Opioid Use Following Outpatient Surgery in Adolescents. BMJ open, 15(4), e099679. https://doi.org/10.1136/bmjopen-2025-099679
Harris, H. W. (2025). Active Inference and Psychodynamics: A Novel Integration With Applications to Depression and Stress Disorders. Frontiers in Psychiatry, 16. https://doi.org/10.3389/fpsyt.2025.1630858
Igunma, C. H., Ohaeri, B., Ojo, I. O., & Babarimisa, O. (2022). Risk Factors Associated With Substance Abuse Among Adolescents. International Neuropsychiatric Disease Journal, 11-24. https://doi.org/10.9734/indj/2022/v18i130214
Ma, H. (2026). Reward Reactivity in Non-Suicidal Self-Injury in Adolescents: Protocol for a Longitudinal Study. https://doi.org/10.21203/rs.3.rs-8267494/v1
Magomedova, A., & Fatima, G. (2025). Mental Health and Well-Being in the Modern Era: A Comprehensive Review of Challenges and Interventions. Cureus. https://doi.org/10.7759/cureus.77683
Mansharamani, H., Mansharamani, B., Behere, P. B., Nagdive, A., & Mansharamani, D. (2023). Personality Traits in Children Of Alcoholic Parents. https://doi.org/10.5772/intechopen.106961
Meier, I. M., Honk, J. v., Bos, P. A., & Terburg, D. (2021). A Mu-Opioid Feedback Model of Human Social Behavior. Neuroscience & Biobehavioral Reviews, 121, 250-258. https://doi.org/10.1016/j.neubiorev.2020.12.013
Mooney, A., Crafti, N., & Broadbear, J. H. (2023). Borderline Personality Disorder, Substance Abuse and Disordered Eating: Perceptions of Treatment and Recovery Within Community Mental Health. The Journal of Mental Health Training Education and Practice, 18(6), 377-396. https://doi.org/10.1108/jmhtep-01-2022-0003
Nath, A., Choudhari, S. G., Dakhode, S. U., Rannaware, A., & Gaidhane, A. (2022). Substance Abuse Amongst Adolescents: An Issue of Public Health Significance. Cureus. https://doi.org/10.7759/cureus.31193
Powell, C. (2021). Caring for the Psychosocial Needs of the Acutely Traumatized Patient. Jaapa, 34(11), 24-29. https://doi.org/10.1097/01.jaa.0000794980.31616.fa
Ramírez, M., Ugedo, A., Fañanás, L., Cano-Escalera, G., Sáiz, P. A., Zorrilla, E. P., & González-Pinto, A. (2025). Scoping Review of Biological and Psychosocial Pathways That Lead From Childhood Adversity to Early-Onset Substance Use. Frontiers in Psychiatry, 16. https://doi.org/10.3389/fpsyt.2025.1612494
Reese, S. E., Conradt, E., Riquino, M. R., & Garland, E. L. (2021). An Integrated Mechanistic Model of Mindfulness-Oriented Recovery Enhancement for Opioid-Exposed Mother–Infant Dyads. Frontiers in psychology, 12. https://doi.org/10.3389/fpsyg.2021.688359
Rezapour, T., Rafei, P., Baldacchino, A., Conrod, P., Dom, G., Fishbein, D., Kazemi, A., Hendriks, V. M., Newton, N. C., Riggs, N. R., Squeglia, L. M., Teesson, M., Vassileva, J., Verdejo‐García, A., & Ekhtiari, H. (2022). Neuroscience-Informed Classification of Prevention Interventions in Substance Use Disorders: An RDoC-based Approach. https://doi.org/10.1101/2022.09.28.22280342
Rizk-Hildbrand, M., Semple, T. J., Preisig, M., Haeberling, I., Smigielski, L., Pauli, D., Walitza, S., Kleim, B., & Berger, G. (2025). The Body as a Battleground: A Qualitative Study of the Impact of Violence, Body Shaming, and Self-Harm in Adolescents With a History of Suicide Attempts. International journal of environmental research and public health, 22(6), 859. https://doi.org/10.3390/ijerph22060859
Rodan, S.-C., Aouad, P., McGregor, I. S., & Maguire, S. (2021). Psilocybin as a Novel Pharmacotherapy for Treatment-Refractory Anorexia Nervosa. OBM Neurobiology, 05(02), 1-25. https://doi.org/10.21926/obm.neurobiol.2102102
Rojas-Jara, C., Polanco-Carrasco, R., Navarro-Castillo, R., Faúndez-Castillo, F., & Chamorro-Gallardo, M. (2022). “Game (Not) Over”: A Systematic Review of Video Game Disorder in Adolescents. Revista Colombiana de Psicología, 31(2), 45-64. https://doi.org/10.15446/rcp.v31n2.90741
Sampedro‐Piquero, P., Zancada-Menéndez, C., Brotóns, E. B., & Moreno‐Fernández, R. D. (2022). The Relationship Between Binge Drinking and Binge Eating in Adolescence and Youth: A Systematic Review and Meta-Analysis. International journal of environmental research and public health, 20(1), 232. https://doi.org/10.3390/ijerph20010232
Sarkingobir, Y., & Tukur, U. (2024). Effects of Drug Abuse on Primary Education: An Overview Context. Jurnal Riset Madrasah Ibtidaiyah (Jurmia), 4(1), 85-95. https://doi.org/10.32665/jurmia.v4i1.2791
Sazhin, D., Frazier, A. M., Haynes, C. R., Johnston, C., Chat, I. K., Dennison, J. B., Bart, C. P., McCloskey, M. E., Chein, J., Fareri, D. S., Alloy, L. B., Jarcho, J. M., & Smith, D. V. (2020). The Role of Social Reward and Corticostriatal Connectivity in Substance Use. Journal of Psychiatry and Brain Science. https://doi.org/10.20900/jpbs.20200024
Sinha, R. (2024). Stress and Substance Use Disorders: Risk, Relapse, and Treatment Outcomes. Journal of Clinical Investigation, 134(16). https://doi.org/10.1172/jci172883
Thapar, A., Eyre, O., Patel, V., & Brent, D. A. (2022). Depression in Young People. The lancet, 400(10352), 617-631. https://doi.org/10.1016/s0140-6736(22)01012-1
Tubbs, A., Fernandez, F. X., Grandner, M. A., Perlis, M. L., & Klerman, E. B. (2022). The Mind After Midnight: Nocturnal Wakefulness, Behavioral Dysregulation, and Psychopathology. Frontiers in Network Physiology, 1. https://doi.org/10.3389/fnetp.2021.830338